The day I left my Doctor’s clinic with my first ever prescription for anti-depressants, was the day I pulled out all the research I could find relating to menopause-related depression, including the role of exercise. I was confused as to why, when I have never had depression in my life, it had arrived during my early 50s. The relationship to menopause and the type of exercise I was doing at the time, never crossed my mind, nor, I imagine, did it cross the mind of my medical practitioner.
That day was pivotal to me. Because it moved me aside from always doing higher intensity exercise, to getting back to doing good old-fashioned aerobic exercise. With the emphasis on high-intensity performance-based activity and weight training, aerobic exercise has been relatively forgotten in the fitness industry.
For women in mid-life suffering from menopause-related depression, this needs to change. How heartening to also hear this from Australia’s Psychiatric academic, Professor Felice Jacka, at an online lifestyle medicine conference I attended recently.

The history of menopause-related anti-depressant use is fascinating. A medication called Iproniazid, developed in the early 1950’s for treatment of tuberculosis, was never intended to become one of the first pharmaceutical anti-depressants.
But when Physician’s noticed that tuberculosis patients became more cheerful, optimistic and more physically active, further research revealed that the change from melancholy to motivation in these patients was due to the slowing down of the enzymes that broke down the two main mood-enhancing hormones, serotonin and dopamine. [Leibermann, 2003]
So began the genesis of anti-depressant pharmacology and alongside the growing interest in psychiatry as a medical discipline in the 1960’s and 1970’s, the use of anti-depressants to help women in menopause cope better with their melancholy, emerged as a treatment of choice.
Throughout the 1970’s, the development of Fluoxetine flourished and this was the first Selective Serotonin Reuptake Inhibitor (SSRI) medication which helped millions of women cope better with everyday life. In the United Kingdom, two-thirds of anti-depressants are now prescribed to women in mid-life.
Anti-depressants interact with receptors located on nerve endings. As such, this interaction changes neural (nerve) functioning and the uptake of our mood hormone serotonin. For someone who has been healthy and happy all her life, it was a confusing time to decide whether to go on these (and I know that they help millions of women, including many women who come onto the MyMT™ programmes).
However, as a researcher in exercise and sports science, I was also aware of the powerful role that exercise plays in our mental health as well. In fact, every one of the women in my doctoral studies, told me that the main reason that they took up exercise over their lifetime, was simply because not only did it make them ‘feel good’, but as they moved into mid-life, it helped them to cope. The problem however, that there was no knowledge of the type and amount of exercise they needed to be undertaking in menopause and many of them were doing daily higher intensity activity. At the time, so was I. But this is not the type of exercise that is best suited to women with changing hormones during menopause and who are exhausted from not sleeping.

How did we get to the point whereby we’ve forgotten about the mental health benefits of endurance exercise, of which women and their cardiovascular system are most suited to? This was one of the questions I asked myself. But as one of many women who helped to pioneer the modern fitness industry in New Zealand, I remember the fitness messages in the 1990’s.
This was the time when ‘lack of time‘ became the new mantra for the fitness industry. In the 1980’s and 1990’s there was a phenomenal growth in jogging, triathlons, women’s events and more. And alongside this movement, grew the Sport and Exercise Science movement, which fueled the increased emphasis for athletes and everyday men and women to get fitter and stronger.
Motivated by the very new scientific domain of exercise psychology, one of the messages coming out of the emerging activity participation research, was that most people lack time to exercise. Alongside these messages, was also the very, new sports science messages, that showed if we want to improve fitness, and when we don’t have much time, then we need to increase the intensity whilst decreasing the duration of the workout.
Those of us working in the fitness industry knew that when lack of time became the excuse for not exercising, we needed to come up with a solution. Hence, workouts became shorter, faster, harder. Not only did we love the endorphins, but we loved the fact that we could get through the workout in as short a time as possible. This enabled us to get on with our day and for many of us, to get back to work.
So began the 30 minute workout paradigm – now packaged up as Boot Camps, CrossFit and other types of high-intensity workouts.
Not much has changed either. When preparing for my session at a recent conference, I came across a brand new 2018 report from the Australian Institute of Health and Welfare, on Physical Activity Across the Life-Stages. Here’s what it states on pg vii:
‘Not enough time’ and health issues remain a barrier for participation in physical activity and exercise. Almost 4 in 10 adults aged 18–64 (37%) reported ‘Not enough time’ or ‘Too many other commitments’ as the main barriers to participating in sport or recreational physical activities. As age increased, ‘Poor health or injury’ was more frequently cited as the main barrier—increasing from almost one-fifth (18%) of those aged 35–44 to almost half (48%) of adults aged 65 and over.*
As busy women, many of us can relate to this statement I’m sure. But here’s the thing. To mitigate this barrier of ‘no time’, the fitness industry continue to promote 30 minute workouts of higher intensity. And that’s great for 1 or 2 workouts a week because there is increasing research to show that higher intensity exercise improves cardio-metabolic health in weight loss research.
This is because the ‘after-burn’ i.e. the 3-4 hours after the higher intensity exercise, is when fat-burning occurs as our body returns to it’s resting metabolic state and our metabolism passes into ‘aerobic’ mode again.
However, for women who aren’t sleeping, too much high-intensity exercise may send women going through menopause into adrenal chaos and exhaustion. Just like over-trained female athletes.
This is because there is a powerful connection between our sleep hormones, thyroid and adrenal hormones and in menopause they can all get out of balance tipping us into menopause-related depression.

This is why, for women transitioning into peri-menopause and out into post-menopause, the importance of aerobic exercise, [i.e. steady-state exercise, up to an hour], needs to return as ‘exercise of choice’. It’s been forgotten for too long and this is partly because research has not kept up with the exercise needs of mid-life women.
When women only do 30 minute workouts of higher intensity on most days of the week, they are not getting the beautiful steady-state ‘aerobic’ activity, that is best for heart health, mental health and helps to reduce arterial stiffness. That’s why for the women who join me on the MyMT™ symptom reduction programmes, whether they are on menopause-related anti-depressants or not, I get them back doing aerobic exercise. Walking or if sore joints allow (I have a joint health module in the programme) is most often the exercise of choice.
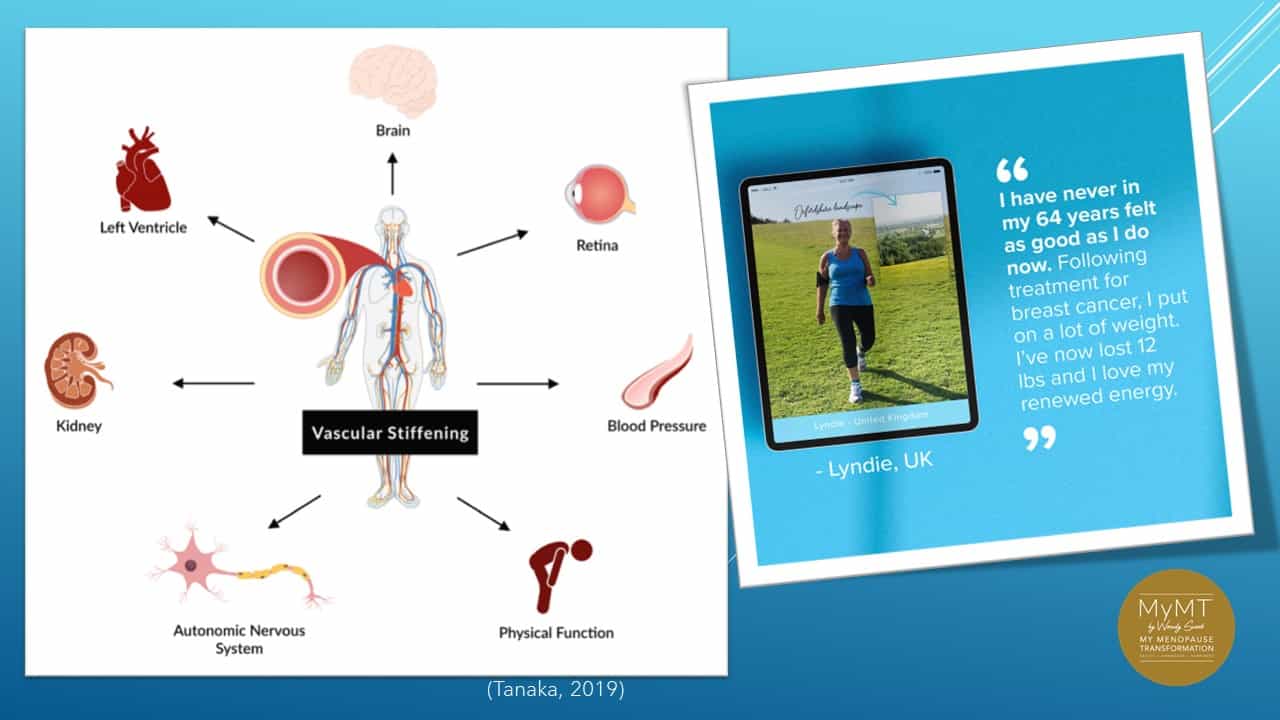
Not only does aerobic exercise help with blood pressure management but it also helps with improving arterial blood flow and reducing vascular stiffness.
The add-on effect with improved blood flow is that aerobic exercise also improves our mental health, through boosting serotonin and dopamine levels – the two hormones of mood management. As we move through menopause, the production of these hormones declines, so aerobic exercise mitigates this.
At the time, I didn’t take the anti-depressants but this was a choice I made with my Doctor. Instead I explored the scientific research on depression, inflammation and exercise specific to menopause. From this research, I also put together a plan to sort out my sleep, gut health, aching joints and food, so that I could return to exercise that mattered to me in menopause and therefore, better suit the ‘change of life’.
When you are ready, I hope you can join me because those same plans are all in the MyMT™ programmes waiting for you too.

References:
*Australian Institute of Health and Welfare (2018). Physical activity across the life stages. Cat. no. PHE 225. Canberra: AIHW.
Doyne, E. et al. (1983). Aerobic exercise as treatment for depression in women. Behavior Therapy, 14(3), 434 – 440.
Firth, J., Solmi, M., Wootton, R.E., Vancampfort, D., Schuch, F.B., Hoare, E., Gilbody, S., Torous, J., Teasdale, S.B., Jackson, S.E., Smith, L., Eaton, M., Jacka, F.N., Veronese, N., Marx, W., Ashdown-Franks, G., Siskind, D., Sarris, J., Rosenbaum, S., Carvalho, A.F. and Stubbs, B. (2020). A meta-review of “lifestyle psychiatry”: the role of exercise, smoking, diet and sleep in the prevention and treatment of mental disorders. World Psychiatry, 19: 360-380. https://doi.org/10.1002/wps.20773
Leibermann, J. (2003). History of the use of anti-depressants in Primary Care. J. Clinical Psychiatry, 5(7), 1-5.

