“Never before has a generation of women been so confused about what to eat! When I take my ‘Masterclass on Menopause’ seminars around the world, I often ask those attending who is confused about their food choices at the moment. Invariably the entire room puts up their hand. I’m not surprised. Because even with my own background teaching sport and exercise science, including nutrition, when I hit menopause, I was confused too.
As the first generation of women to go into menopause in the context of the modern fitness and sporting industries, the dieting industry and our constant exposure to food-advertising over the past few decades, it’s little wonder that we get confused. But herein lies the problem – many of the popular food messages are not researched against women’s health and our changing hormonal environment during menopause. Especially when it comes to carbohydrates. So if you haven’t made the connection between your hot flush frequency and severity and the type of carbohydrates you are eating, then please read on!”
[Dr Wendy Sweet, PhD/ Women’s Healthy Ageing Researcher].

When you begin your peri-menopause transition, you are entering the next stage of your biological life – your ageing years. This is why your reproductive hormones, oestrogen and progesterone, start to decline.
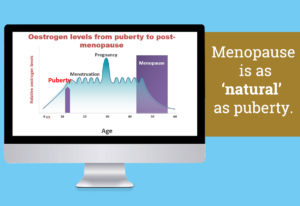
But as I explain in my programmes, when some hormones change in the body, this sets up a ‘chain-reaction’ whereby other hormones try to rebalance the internal environment. Hormones are our chemical messengers and they are all connected, working hard together to keep our body healthy.
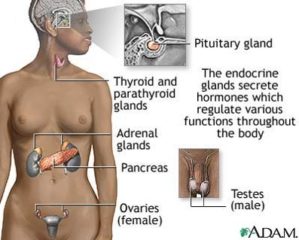 Our endocrine system – the pancreas, thyroid, parathyroid and adrenal glands – is a complex system. These glands produce and regulate many of the hormones that help your body function every minute of every day. And they all work in harmony because they all ‘talk’ to each other. It’s because of this connection that we arrive in menopause and we experience so many symptoms that can be linked to our heart, our muscles, our thyroid, our stress levels, our pituitary function, joint health and more! Most women don’t understand that the symptoms that suddenly come on during menopause, such as sore joints, changing gut and cardiac health, increased anxiety, mood swings, sore muscles, night sweats, insomnia and hot flushes are all connected. But there’s another reason too – we are a unique generation in that we have had a lot of stress throughout our lives, not only emotional, but also physical stress from not sleeping, changing food choices and for many of us, we’ve come through the fitness and sports industries, so we have done a lot of exercise which also increases the internal physical stress on muscles and joints. Add to this the hormonal changes in menopause and not sleeping, our inflammation increases inside our body. The result for many of us, is changing heat regulation too – and our food choices have a lot to do with this too.
Our endocrine system – the pancreas, thyroid, parathyroid and adrenal glands – is a complex system. These glands produce and regulate many of the hormones that help your body function every minute of every day. And they all work in harmony because they all ‘talk’ to each other. It’s because of this connection that we arrive in menopause and we experience so many symptoms that can be linked to our heart, our muscles, our thyroid, our stress levels, our pituitary function, joint health and more! Most women don’t understand that the symptoms that suddenly come on during menopause, such as sore joints, changing gut and cardiac health, increased anxiety, mood swings, sore muscles, night sweats, insomnia and hot flushes are all connected. But there’s another reason too – we are a unique generation in that we have had a lot of stress throughout our lives, not only emotional, but also physical stress from not sleeping, changing food choices and for many of us, we’ve come through the fitness and sports industries, so we have done a lot of exercise which also increases the internal physical stress on muscles and joints. Add to this the hormonal changes in menopause and not sleeping, our inflammation increases inside our body. The result for many of us, is changing heat regulation too – and our food choices have a lot to do with this too.
What are hot flushes?
A hot flush is the body’s attempt to cool you down. It’s trying to get rid of heat. Just like sweating in athletes or when you have a fever. When our body is hot, then we sweat more. But as we come through menopause our sweat glands don’t function as well in a low oestrogen hormonal environment, so we need to turn down the heat in other ways too. This includes changing type of carbohydrates you are eating.
 Whether it’s summer or winter where you live, reducing your hot flushes means managing your hormones that control your blood sugar levels on – insulin and glucagon. High blood sugar causes your pancreas to produce more insulin and when insulin levels are high our heat regulation is affected too. So, if you are going into your menopause years and you are finding that your hot flushes are out of control both day and night, then you need to eat for your age and stage and keep the production of insulin low. High insulin levels in menopause, on top of not sleeping and changing muscle density, sends your inner temperature soaring. It’s also why the MyMT™ programmes only focus on you in your menopause transition. We are in a unique stage of our lives.
Whether it’s summer or winter where you live, reducing your hot flushes means managing your hormones that control your blood sugar levels on – insulin and glucagon. High blood sugar causes your pancreas to produce more insulin and when insulin levels are high our heat regulation is affected too. So, if you are going into your menopause years and you are finding that your hot flushes are out of control both day and night, then you need to eat for your age and stage and keep the production of insulin low. High insulin levels in menopause, on top of not sleeping and changing muscle density, sends your inner temperature soaring. It’s also why the MyMT™ programmes only focus on you in your menopause transition. We are in a unique stage of our lives.
 Have you noticed that your hot flushes increase with certain foods or fluids? The women on the MyMT programmes understand this very well. When they come on board with me, they learn the powerful connection between all of our hormones in menopause and the role each plays in our hot flushes, poor sleep, low energy levels, sore joints and more. When the same symptoms happened to me and supplements and medications weren’t resolving all of my symptoms, I began to look at our hormonal system and how menopause impacted on the role of other hormones too. Making this connection was a game-changer for understanding how we can better manage our nutrition in menopause to reduce the frequency and intensity of our hot flushes.
Have you noticed that your hot flushes increase with certain foods or fluids? The women on the MyMT programmes understand this very well. When they come on board with me, they learn the powerful connection between all of our hormones in menopause and the role each plays in our hot flushes, poor sleep, low energy levels, sore joints and more. When the same symptoms happened to me and supplements and medications weren’t resolving all of my symptoms, I began to look at our hormonal system and how menopause impacted on the role of other hormones too. Making this connection was a game-changer for understanding how we can better manage our nutrition in menopause to reduce the frequency and intensity of our hot flushes.
Although I have an entire 40 minute webinar on the specific lifestyle solutions to put into place to turn around your hot flushes (whether you are in menopause or post-menopause), I’m always updating women in the programmes on how they can better manage their hot flushes by not only improving their sleep, but also changing their diet and their exercise to better match their changing hormonal environment in menopause.

Women read these updates and posts in my private coaching community which is another part of the MyMT programmes. One of these topics was about sugar and starch and why the intake of too much of these foods have such an impact on our hot flushes in menopause (as does too much exercise, being overweight, feeling stressed and not sleeping).
Maybe you have discovered that high sugar and certain carbohydrate foods contribute to your hot flushes too? I still remember the surprise of making the connection between my intake of sugar and refined carbohydrates and how this caused an almost immediate surge of heat through the body followed by excessive sweating. Feeling hot and sweaty at all hours of the day and night is so frustrating and exhausting.
Which is why I drew on my physiology knowledge and made the connection between high insulin levels, our diet and our temperature regulation in menopause.
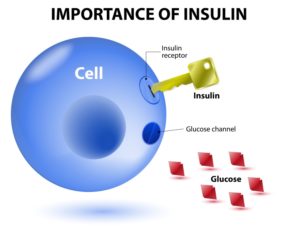
I knew from my sports nutrition teaching that athletes need certain high glucose (sugar and starch carbohydrates) foods that cause a surge of the hormone insulin to be released from the pancreas. Insulin is the hormone which helps to carry glucose to muscle cells quickly, so as to keep the muscles contracting for long periods of time. When the muscles deplete their stores of glucose, then the liver kicks in to rectify the situation and helps to produce more glucose ready for the muscles to keep using. Glucose is moved around the body by a hormone called Insulin. It’s role is crucial to our survival, because glucose is needed by almost every cell in the body, especially our brain, liver and muscle cells.
So, how do foods that contain sugar and refined starch cause more hot flushes? That’s the question I asked myself because I could feel this happening to my body. The response of heat was almost immediate when I ate sugar or had alcohol, so I knew there was a link.
This led me to look at insulin and the connection with our body temperature. It was only in 2010 that researchers from Scripps Clinic* in San Diego, who were researching diabetes, found a link between high insulin levels and body temperature. The study showed that when the hormone, insulin, stays high in the blood stream, there is a direct connection with dilation of blood vessels and heat production in the brain and ‘core’ organs (these are your major organs in the trunk). The study also found that variations in core body temperature are associated with our daily 24-hour sleep-wake cycle, the female monthly hormonal cycle, and, intriguingly, the effects of very severe calorie restriction such as all-day fasting which increases heat production in the body too. [It’s also why I teach the importance of nutrient timing to women on my programmes and overnight fasting, but not fasting during the day. This is really helpful to women on the Transform Me weight loss programme. When we fast overnight our insulin levels decrease and so too does our stress hormone called cortisol].
Understanding the powerful link between our hot flushes and our temperature regulation is what led me down the path of recommending Low Glycemic Index carbohydrates as one of the strategies I teach women on the MyMT programmes to control their hot flushes. [There are other powerful strategies to reduce hot flushes in the programme too, especially around nutrient timing and exercise timing].
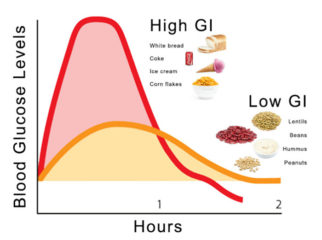 Low Glycemic Index is the name given to certain carbohydrates, or energy foods that don’t spike high insulin production from the pancreas. We have Professor Jennie Brand-Miller from the University of Sydney in Australia, to thank for her incredible work on the glycemic index rating of carbohydrates. When we eat foods that are Low GI, then we don’t release as much insulin and therefore, don’t get the high heat production either. This is why I have low GI food lists in my specially designed MyMT Eats Cookbook which women access as part of the MyMT programme. There is also an Australian website you can visit called www.gisymbol.com
Low Glycemic Index is the name given to certain carbohydrates, or energy foods that don’t spike high insulin production from the pancreas. We have Professor Jennie Brand-Miller from the University of Sydney in Australia, to thank for her incredible work on the glycemic index rating of carbohydrates. When we eat foods that are Low GI, then we don’t release as much insulin and therefore, don’t get the high heat production either. This is why I have low GI food lists in my specially designed MyMT Eats Cookbook which women access as part of the MyMT programme. There is also an Australian website you can visit called www.gisymbol.com
The foods that cause the MOST insulin production and release from the pancreas are:
1. Sugars – Sucrose, Glucose & Lactose are the most common forms of sugar. Sucrose is also known as common table sugar and is made up of glucose and fructose. Lactose is the sugar found in milk and is made up of glucose and galactose. Fructose is the sugar found in fruit (and fruits are still important in our diet, but I have a list of low GI fruits that are best for us in menopause). There are many other sources of sugar too – for example, dextrin, maltose and maltodextrins! (Milo anyone or what about all that chocolate milk promoted by sports stars and athletes?!)
If we are exercisers, then we do need some sugar in our diet as this is very quickly taken up by muscles and our brain. But not all sugars are equal. For example, dried fruit are easily digested as are apples, which are low GI fruit. Bananas are higher GI so this is a great source of starch which is broken down to glucose, and having this before or after exercise will help replace glucose into muscles. You must also remember that commercial sports drinks are just sugar in disguise, so if you are doing lots of exercise, then stick with water and some easily digested fruit to help you recover from your exercise. I have the specific solutions in both of the MyMT programmes and in my ‘Rebuild My Fitness’ programme which teaches you all the information you need for your exercise.

2. Starches are important to understand too and these are not always equal either. Remember that there are man-made starch foods and natural starch foods. Natural starches occur in vegetables. Starches (formerly known as complex carbohydrates) occur naturally in a large range of foods including nutrient-rich foods like root vegetables, legumes, cracked wheat, brown rice, pearl barley, quinoa and oats. But starch is also found in refined products such as cornflour, white bread, many breakfast cereals, potato crisps, French fries, rice crackers/cakes, biscuits, cakes, and pastries. These are refined starches and aren’t good for our health or hot flushes, so keep these to a minimum and increase your vegetable carbs which are lower GI.
The most important starch for women is RESISTANT STARCH.
Resistant Starch is another type of dietary fibre. It’s actually a starch that ‘resists’ digestion and absorption in the small intestine and travels through the large intestine largely intact. It ends up in the small intestine where it is fermented into short chain fatty acids by good bacteria. There is strong evidence that resistant starch is important for our health as we age, which is why we need a bit more focus on it at this stage of life along with vegetables which provide you with important fibre to help control insulin levels too.
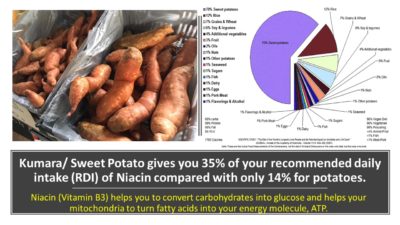
 Resistant Starch is found mostly in beans, lentils, unripe bananas as well as unprocessed cereals and wholegrains. Resistant starch is also created from cooling down cooked rice, potatoes, kumara (sweet potato) and other root vegetables.
Resistant Starch is found mostly in beans, lentils, unripe bananas as well as unprocessed cereals and wholegrains. Resistant starch is also created from cooling down cooked rice, potatoes, kumara (sweet potato) and other root vegetables.
I think the greatest realisation for me when I was trying to understand why I was having so many hot flushes, was that food type and timing also matters.
I used to eat lots of high sugar and starch foods which my body craved, because for decades, I was doing a lot of higher-intensity exercise and this was contributing to my sugar cravings. My brain and muscles continually wanted glucose! Then as life got busy and peri-menopause came along, I was less active but was still in the HABIT of eating carbs that caused this insulin spike. Before menopause arrived, I probably didn’t even notice the heat connection! It took a lot of determination to turn this around and I’m so thankful for my Masters studies into lifestyle behaviour-change strategies, because not only did I have to use these strategies on myself, but how to change our behaviour and habits has become an important component of the MyMT programmes. I encourage all of the women on the programmes to think ahead, planning and preparing foods that reduce hot flushes and keep blood sugar levels stable. How to achieve this important aspect of our menopause management is all in both of the MyMT programmes.
Carbohydrates are really important to us in menopause because they are our source of energy. So, if I hear fitness and nutrition practitioners talking about a ‘low-carb’ diet, then I walk away from them because it means that they don’t understand nutrition or hormonal physiology!
 Vegetables are the most important carbohydrates on the planet and we need them for our health during menopause and into our years beyond.
Vegetables are the most important carbohydrates on the planet and we need them for our health during menopause and into our years beyond.
But all carbohydrates are not equal and as the first generation of women to come into menopause in the context of our changing food environment, many of us are addicted to a high sugar and processed starch diet. This needs to change when we reach menopause and it’s why I want to help you achieve this. Our brain has powerful hormones which keep us addicted to sugars if we don’t learn strategies to turn this around. This is why I have researched the exact carbohydrates that cool you down, not heat you up! If you are already overweight or putting on belly-fat, then this higher fat level changes your insulin levels too – that’s why overweight women typically get more hot flushes.
 If this is you and you are stacking on the weight, then when you are ready, come join me on my menopause weight loss specific ‘Transform Me’ programme. Losing weight will help you reduce your hot flushes and night sweats too.
If this is you and you are stacking on the weight, then when you are ready, come join me on my menopause weight loss specific ‘Transform Me’ programme. Losing weight will help you reduce your hot flushes and night sweats too.
 Otherwise, if you aren’t overweight, then join me on my Circuit Breaker programme. I can’t wait to meet you and support you to make the lifestyle changes that you need to make as you transition into the next phase of your life. As I say to women, there’s no looking back to the past. It’s all about looking forward to our healthy ageing years ahead and all the excitement that is still to come.
Otherwise, if you aren’t overweight, then join me on my Circuit Breaker programme. I can’t wait to meet you and support you to make the lifestyle changes that you need to make as you transition into the next phase of your life. As I say to women, there’s no looking back to the past. It’s all about looking forward to our healthy ageing years ahead and all the excitement that is still to come.
Wendy Sweet, PhD/ MyMT Founder – [Meet me HERE]
[* Sanchez-Alavez et al. (2010). Insulin causes hyperthermia by direct inhibition of warm sensitive neurons. Diabetes. 59(1): 43-50.]

