Will combining this diet with the right exercise reduce cholesterol and blood pressure in post-menopause?

When forty obese post-menopausal women in Cairo , aged 50-60 yrs participated in a study exploring the effect of diet and exercise on their cardiovascular health, they would have had no idea how influential it might be on many of us here in my newsletter community. In a shout-out to these women and the researchers, […]
Your ageing arteries in post-menopause and the magic of magnesium.

Women’s health and ageing research is replete with cardiovascular disease studies. The declining health of our mother’s generation have paved the way for this type of research in older women. For many women, menopause is the start of their changing heart health … but here’s the thing that our mother’s generation didn’t know – it doesn’t […]
Making Waves: The benefits of cold-water swimming for your heart health and weight management in post-menopause.
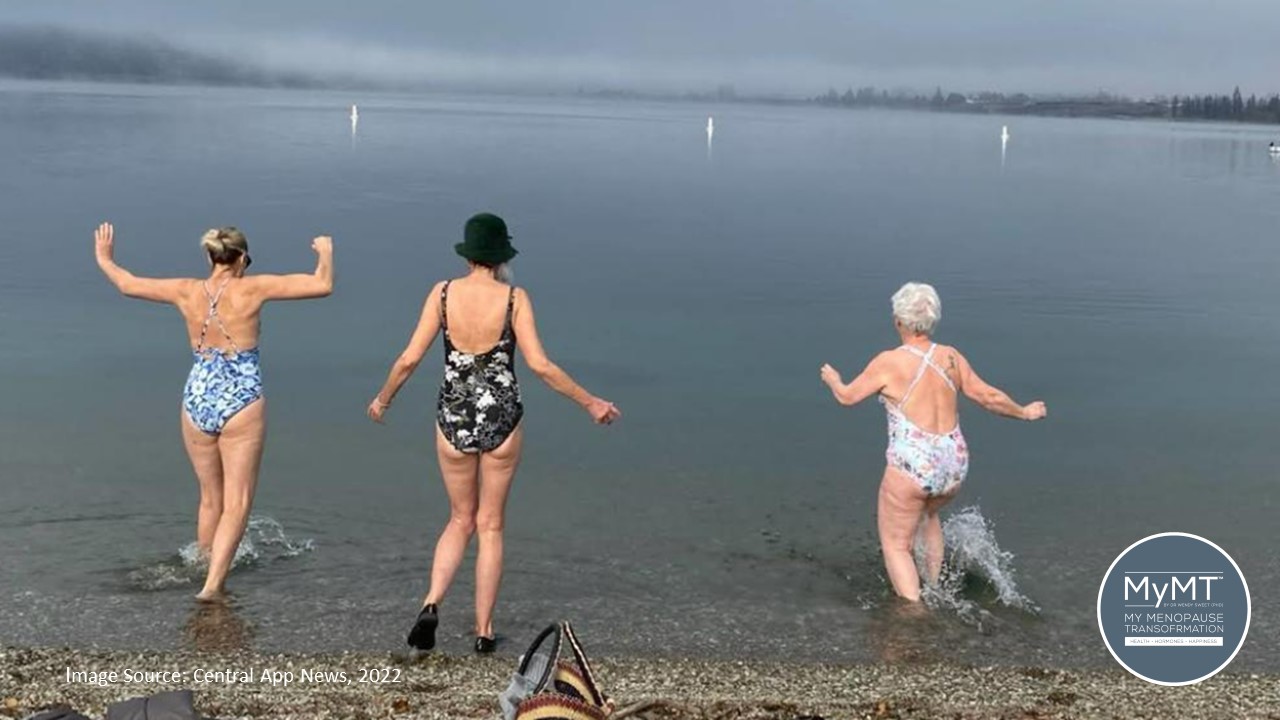
Over the past few days, in a small New Zealand South Island town, swimmers have been brvely swimming length after length in an outdoor pool. If you think that this is not an unusual phenomenon, then let me explain … the water temperature in the pool has met the International Ice Swimming Association (IISA) regulation […]
The month of July is the MyMT™ POST-MENOPAUSE Transform Me weight loss sale

For the first time ever I have a promotion aimed at women in post menopause. As part of my focus on the last of the Baby-boomer generation and the first of the Gen-X women, I’m adding in a brand new module on women’s heart health. Heart health continues to be the number one health concern […]
Wild Yams for Post-Menopause Hot Flushes – what the science says.

If you’ve walked into your pharmacy or health supplement shop lately and cast your eyes over the plethora of menopause-related supplements and creams, you might have noticed that the ingredients list mentions wild yams. Or perhaps you are taking your ‘bio-identical’ hormone replacement therapy (HRT) and when you look at the ingredients, they mention wild […]
“I’m slimmer, healthier and full of gratitude for your MyMT™ programme.” – Bev Rhodes

“Before I began this programme I was exhausted and overweight. You made my decision to look after myself so much easier with the research you have completed and put into this programme. There is much I want to fit in to the rest of my life still and now I feel I have the energy […]
