Why have women become so busy and stressed, that this is now affecting their hormonal balance?
The concept of the Stress Adaptation Response was first conceptualised in the 1950s by Psychologist, Dr Hans Selye.
Since his early research and descriptions of the ‘General Adaptation Syndrome’ (G.A.S.), this syndrome has been seen as a three-stage process of (1) alarm reaction, (2) adaptation stage, followed by chronic stress and (3) the exhaustion stage.
But whilst these stages are well known, researchers now better understand that there is so much more going on in terms of the physiological and emotional responses to stress, as well as the effect on the HPA-Thyroid Axis in women.
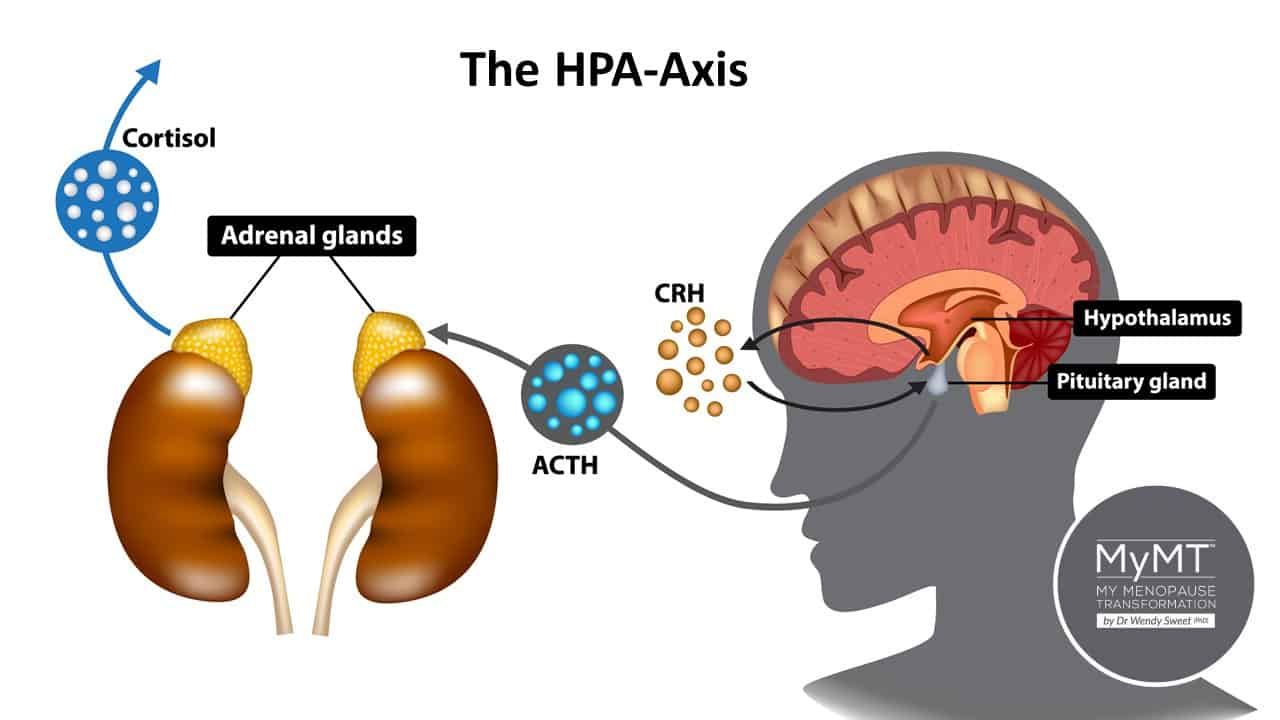
The HPA-Thyroid Axis refers to the powerful bio-chemical connections that exist between the hypothalamus, pituitary, adrenal and thyroid glands.
They are key regulatory centres in the body and their respective hormones are influenced by numerous genetic, environmental and developmental factors. As such, many of these hormones get out of balance as we move through life.
For example, imbalances of the HPA-Thyroid Axis are easily triggered by grief, fear, anxiety, excitement, sleep disorders, blood glucose dysregulation, inflammation, low nutrient absorption and of course, by our changing hormonal profile as we move through menopause into post-menopause.
Changes to ovarian function during menopause influence the balance of the HPA-Axis and it’s normal regulation too.
This normal regulation and balance of our hormones is known as ‘homeostasis’. This is the state whereby the organs and hormones as well as the bio-chemistry of the body are continually changing and adjusting to sources of stress (stressors) in order to maintain balance within the body.
There are many events which alter homeostasis, and for women feeling stressed, these events may be physical, chemical and emotional/ personal.
Over 20 years ago, I used to give numerous talks to workplaces on stress, fatigue and wellbeing. I used to show attendees the graph below.
It depicts how athletes, when training, undergo an increased workload to stimulate positive performance changes, and then afterward the gruelling training sessions, they focus on their recovery. Work and recovery – this is how athletes improve performance.
If they don’t get the balance right, then it may be that they are over-training. As such, there is a period of ‘diminishing returns’ – a known phenomenon in sports science, whereby health changes occur, especially in female athletes, whereby their HPA-Thyroid Axis gets out of balance … as does their hormone balance.
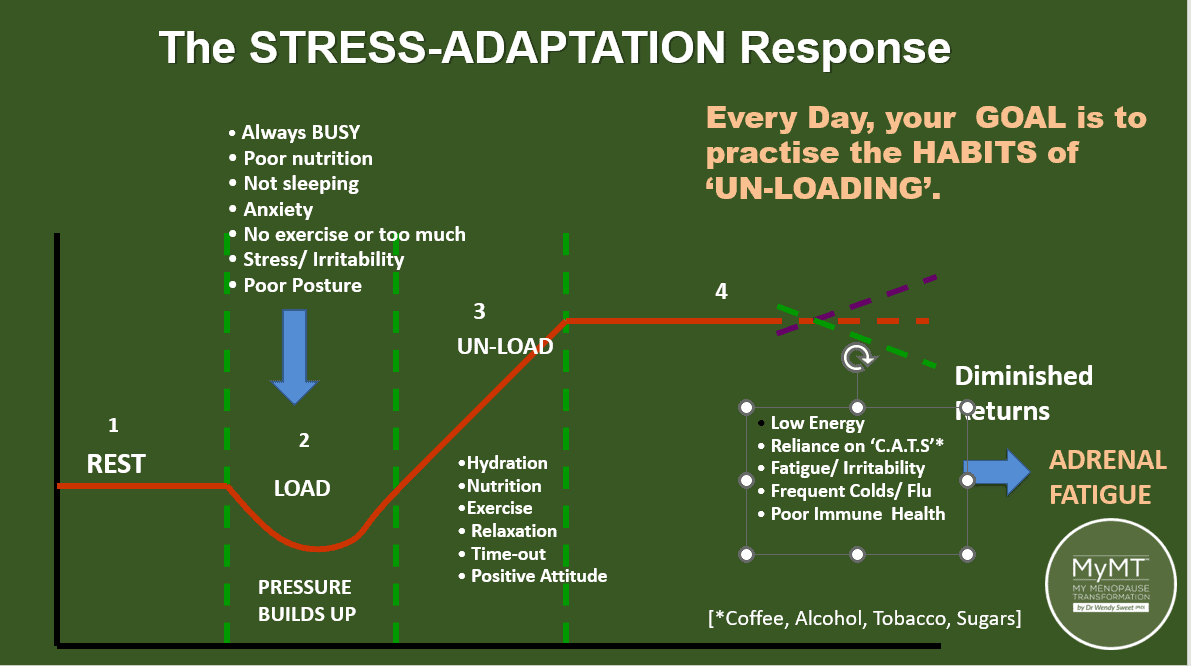
As I explained to the Health Professionals on my CPD course this week, the concept of ‘too much daily load’ and ‘not enough unload’ is the same for women in peri-menopause and menopause.
Many women these days are feeling busy, time-poor and physically and emotionally stressed. Their body and their hormones are under ‘load’ and as such, if they aren’t recovering well, or resting, or eating the right nutrients, then the HPA-Thyroid Axis is working harder to try to restore balance.
But here’s what happens when we are stressed and the HPA-Thyroid Axis is out of balance – women typically go into ‘coping mode’.
For some women, this means they eat more, or eat less. Perhaps they exercise more, or experience changing moods, from melancholy to anger or they begin to feel anxious. Sometimes, they experience physical symptoms, such as sore joints and aching muscles.
Often, they feel hot and experience poor sleep and night sweats. For many, their caffeine, alcohol, tobacco or sugar consumption increases too – you can see in the diagram that over 20 years ago, I called these ‘C.A.T.S.’. Yes, it was the same back then as it is now.
When various sources of stress build up, menopause symptoms become worse. This increase in stress-sources is known as ‘allostatic load’ and for women, there are a variety of sources of stress. I wonder how many you can list!
As sources of stress accumulate, the effect on the body may lead to burn-out and exhaustion. Performance and motivation declines which can then lead to ‘diminished returns’, i.e. changing immune health (frequent colds and flus), changing thyroid function (feelings of heightened anxiety, hot or cold feelings and low energy) and changing pituitary function (poor sleep patterns).
I wonder if all this sounds familiar?

The more stressed we feel, the higher is our production of a chronic stress hormone called cortisol.
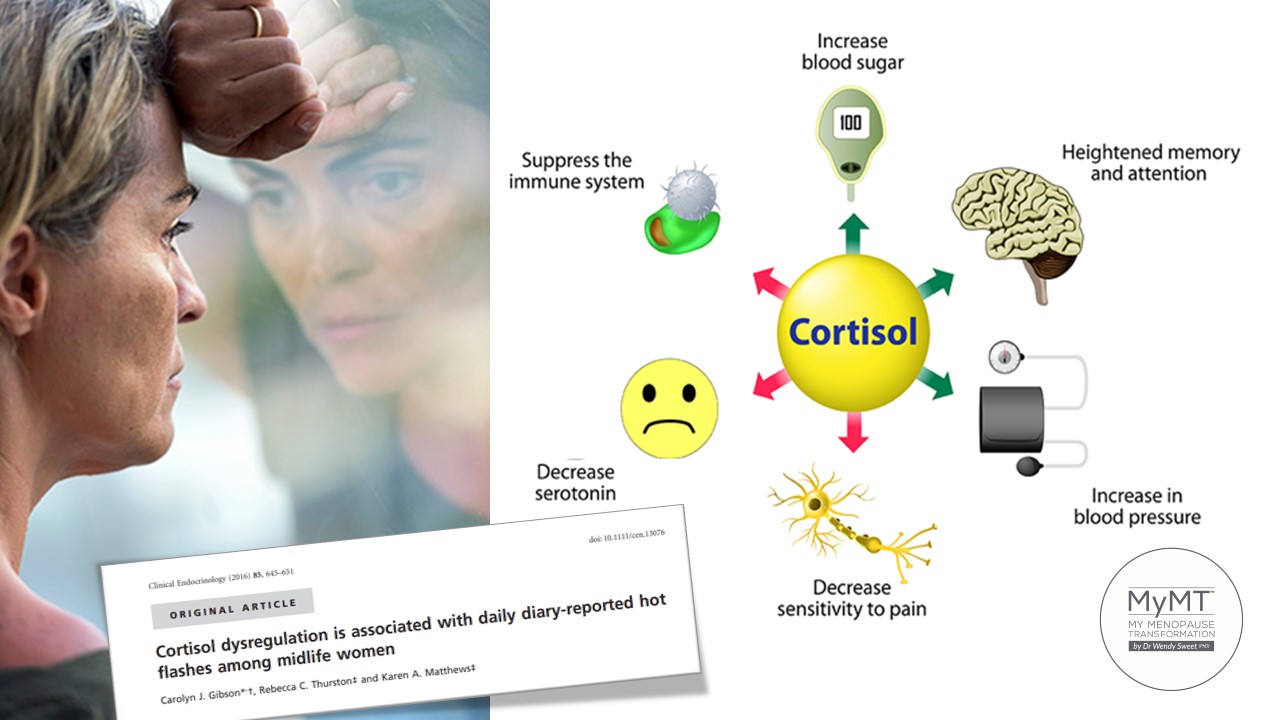
Our chronic stress hormone, Cortisol, is a pesky hormone.
As one of our stress hormones produced by the adrenal glands, balancing cortisol production as the day goes on is important. It has far-reaching effects around the body — including your muscles and bones, heart and blood vessels, lungs, hormone-producing glands, liver, gut and your brain. Some cortisol production is good, but too much over a long time starts to impact our health.
For example, high levels of cortisol can lead to weight gain. Cortisol has an intricate relationship with the hormone insulin, which controls our blood sugar. High or low cortisol can cause hypo-glycemia (low blood sugar), hyper-glycemia (high blood sugar) or both.
When cortisol levels increase, the cells of our body can become resistant to insulin, the hormone that regulates blood sugar levels. This may lead to an increase in blood sugar, weight gain and potentially Type 2 Diabetes as women head into post-menopause when periods have ended for a year or more.
High levels of cortisol may also disrupt the other hormone-producing glands, such as our pituitary gland which produces melatonin, our thyroid gland which helps to regulate temperature and metabolism and when cortisol levels are high, then this can also disrupt the balance between oesterogen and progesterone.
With this disruption, we can also lose the protective role of calming progesterone. If you are feeling bloated, tired, wired, angry, frustrated and experiencing sore breasts or loss of hair too, then you will know what I mean about low progesterone.
If you’ve been experiencing an increased heart rate, anger, frustration, memory lapses and/or hot flushes and night sweats, then, as women on the MyMT™ programmes discover, it’s time to manage your production of cortisol.
When cortisol is out of balance and it stays high throughout the day and night, then your menopause symptoms may become worse. As the Seattle Midlife Women’s Health Study (2009) suggests,
“Rising cortisol levels have been associated with poor health, including lower bone density in older women, minor cognitive complaints, and could be hypothesized to be related to perceptions of poor health overall.” (p. 2).
When I went into peri-menopause, the time of our lives when our ovaries gradually stop producing oestrogen and our progesterone declines as well, I had no idea that not sleeping all night as well as the type of exercise I was doing, was connected to my night sweats, hot flushes and mounting feelings of daily stress, anxiety, brain-fog and fatigue.
Like thousands of women going through menopause, I felt emotionally and physically exhausted but boxed-on – as we tend to do when there is so much to be done. Like so many other women heading into post-menopause, the weight just crept up and up, despite exercise and dieting.
Emotional and physical stress are accumulative – and it’s not just the ‘here and now’ stress. I’m also talking about the decades-long build-up of oxidative or physical stress that manifests as inflammation and metabolic chaos in our body too.
If your muscles are sore, if you have fibromyalgia, if your gut health has changed, if you have put on weight, and if you are feeling hot and bothered all the time, and you aren’t sleeping, then yes, these are all signs that your body is ‘stressed’.
Identifying the Sources of your Stress is Important to your Symptoms
What are the sources of stress impacting you? Are you doing too much exercise, or not enough? Do you sleep all night? Do you feel that you are time-poor juggling both workplace and family demands? Perhaps you are caring for elderly parents as numerous women on my programmes are doing too?
To manage symptoms in menopause and to improve your health as you age, you need to address these sources of stress. I can’t reinforce this enough. And there’s another reason for this.
Oxidative or cellular stress and high levels of cortisol production are becoming well recognised as a cause of age-related diseases due to chronic inflammation.
This chronic inflammation arrives in our gut, liver, heart and kidneys as well as muscles and joints as we age. And yes, the brain doesn’t escape the effects of damaged and inflamed cells and tissues either.
In a new study about the brain and stress, the authors state,
‘Allostatic load represents the ‘wear and tear’ of chronic stress on the brain and body and … women show gender-specific variation for numerous factors such as age, race/ethnicity, adversities and health behaviours, that influence associations between allostatic load and their mental health.’ (Kerr, Kheloui, et el., 2020, p.1).

Build your Resilience to Managing Stress Levels in Menopause:
Health and wellbeing in later life is not just about maintaining physical and mental health, but also about creating an environment that enables us to live our life to the full.
With the world going into a huge age shift, the United Nations announced in 2020, that they were naming 2020 to 2030, the Decade of Healthy Ageing. Our ageing starts during our menopause transition. As such, women particularly, need to focus on their cardiovascular health in order to start to build their stress-resilience.
Since 1980, the American College of Cardiology (ACC) and American Heart Association (AHA) have translated scientific evidence into clinical practice guidelines with recommendations to improve cardiovascular health. Fortunately, these guidelines now look at both men and women differently. This is important.
Women age differently to men, especially when it comes to cardiovascular health and stress. Declining oestrogen levels impact the elasticity of blood vessels and this can lead to a condition called vascular stiffness which I’ve spoken about in other articles.
With this in mind, one of the main things we can do, to begin building our resilience is to do some exercise – but not just any exercise! To help reduce the effect of vascular stiffness, we need to focus on simple, aerobic exercise.
There is a dose-response relationship between Cardiovascular Disease and aerobic physical activity. Even 1 hour of walking per week is associated with lower risk, but the ideal is 150 minutes of aerobic exercise per week, as your starting point for improving heart health and lowering your stress levels.
Aerobic exercise helps your circulation and helps to dilate your blood vessels. All necessary factors in reducing blood pressure as our other preventative measures such as reducing your cholesterol levels, losing weight if you are overweight (especially reducing belly fat and getting your waist circumference under 84 cm) and of course, stopping smoking and eating a diet evidenced for cardiac health as I have for you in the MyMT™ programmes.

It’s never too late to turn around your health as you age. How to achieve this in a step-by-step progressive way is in the MyMT™ programmes, whereby I use scientifically-evidenced lifestyle solutions to help you manage your symptoms – no matter what other treatments you are on, you need these lifestyle solutions too.
12 weeks might just change how you are feeling and most importantly, set you up for your healthy ageing years ahead.
Dr Wendy Sweet (PhD)/ Member: Australasian Society of Lifestyle Medicine.

References:
Childs, E., & de Wit, H. (2014). Regular exercise is associated with emotional resilience to acute stress in healthy adults. Frontiers in Physiology, vol. 5 161. 1, doi:10.3389/fphys.2014.00161
Davis, S., Castelo-Branco, C. et.al. (2012). Understanding weight gain at menopause. Climacteric, 15: 419–429.
Kerr, P., Kheloui, S. et al. (2020). Allostatic load and women’s brain health: A systematic review. Frontiers in neuroendocrinology, Vol 59, 100858,
Stewart, A.L., Kathawalla, UK., Wolfe, A.G. et al. (2018). Women’s heart health at mid-life: what is the role of psychosocial stress?. Womens Midlife Health 4, 11. https://doi.org/10.1186/s40695-018-0041-2
Tanaka H. (2019). Antiaging Effects of Aerobic Exercise on Systemic Arteries. Hypertension, AHA doi: 10.1161/HYPERTENSIONAHA.119.13179.
Woods, N. F., Mitchell, E. S., & Smith-Dijulio, K. (2009). Cortisol levels during the menopausal transition and early postmenopause: observations from the Seattle Midlife Women’s Health Study. Menopause (New York, N.Y.), 16(4), 708–718. https://doi.org/10.1097/gme.0b013e318198d6b2


