2/3 of those on antidepressants in the UK, NZ and Australia are female, and typically in their 50s and 60s.
Why is depression so prevalent in women? This was a question posed by researchers in Canada (Albert, 2015) and one that I have often thought about too. But not just any women – those in mid-life. The prevalence of major depression is higher in women than in men and here in New Zealand, we are in the top-10 of countries to have the highest rate of antidepressant use in the western world. It is higher in women and the rate of prescriptions increases with age. (Bowden, Gibb et al, 2019). Serious stuff.
I was offered antidepressants myself. At the time, I had no idea that going into menopause was a vulnerable time for my mental health. However, I was curious as to why, when I have no history of depressive incidents nor post-partum depression (both factors in menopause-related depression), as to why I not only felt emotionally all over the place, but why my Doctor wanted to put me on them.
Since setting up MyMT™, I’ve read hundreds of pre-entry screening forms, where women indicate that they are taking HRT, Bio-identicals, Anti-depressants and anti-anxiety medications for their menopause symptoms. Whilst I never interfere in this with women because these are all powerful medications that need to be monitored by their medical specialists, what intrigues me the most is that they still report experiencing hot flushes, insomnia, anxiety, brain fog and depression. It doesn’t go past me that these medications are not necessarily working for them, especially as they move into post-menopause. I became curious as to why.
The conclusion I come to time and time again, is that menopause symptoms aren’t being looked at through the lens of our biological ageing. I’m not just talking about our changing reproductive hormones either. There are numerous physical changes that go on inside our body at this time too. These changes occur when oestrogen and progesterone naturally decline and exert influences on the deep tissues and cells that make up every structure in our body. This includes our digestive system and colon.
For millions of women around the world, menopause means poor sleep, hot flushes, worsening anxiety, brain fog and feelings of depression. But there’s also another symptom that isn’t often associated with menopause, nor is it associated with our anxiety, depression and foggy brain.

And that’s the changing health of our gut and digestive system.
So, how is your gut health? Do you suffer from Irritable Bowel Syndrome (IBS)? Or diverticulitis? Or do you swing between being constipated and having diarrhea? Maybe your brain feels foggy all the time and you find it difficult to concentrate? And perhaps these changes have just come on during your menopause transition but you have no idea that they might be connected in some way?
If you feel like this, then you aren’t alone.
At least 50% of women on my coaching pages, tell me that they are experiencing gut health issues that have mainly arrived since they went into their menopause transition. Unbeknownst to many of them, our changing gut health as we go into a low oestrogen hormonal environment is impacting on anxiety levels too.
‘The increase in GI symptoms around the time of menses and early menopause occurs at times of declining or low ovarian hormones, suggesting that estrogen and progesterone withdrawal may contribute either directly or indirectly’ mentions a 2009 study into the role of reproductive hormones on gastro-intestinal symptoms.
But there’s something else impacting on our gut health as well and I have Australia’s Professor Rosemary Stanton to thank for my lightbulb moment. When I heard Professor Rosemary Stanton talk at last year’s Lifestyle Medicine conference in Australia, my ears pricked up:
“After 4 generations of a low-fibre diet since modern food processing arrived in the 1960’s & 1970’s, the gut microbiota has changed to the extent that it no longer supports our immune health. Never before have we seen so much chronic disease caused by the western diet. Diversity in vegetables has the single greatest influence on the gut microbiota. The Mediterranean way of eating is the way to turn this all around.”
The link between your changing oestrogen levels and your gut health could well be the cause of your menopause bloating, IBS or leaky gut. I explain why this is, and the role that oestrogen plays in the integrity of our gut wall, in the video below.
As I explain to women who come on board with the online My Menopause Transformation 12 week programmes, not only are we are the first generation to come into menopause having experienced so many changes to our food environment, but we are also the first generation to have been exposed to harmful substances that have a negative effect on our gut bacteria – and according to researchers, one of the greatest influences on our gut health that has lead to negative gut changes, has been our exposure to antibiotics.
The gut microbiome is one of the largest organs in the body (along with our skin) but here’s what blew me away – when I attended the Australasian Society of Lifestyle Medicine conference late last year, researcher, Professor Thomas Borody, reported that the gut is responsible for producing 70% of your energy. With the powerful connection that your gut has with your brain, many symptoms that we experience in menopause, such as foggy brain, depression, anxiety and mood swings, can be linked to the health of your gut micro-biome. I might also add insomnia in there too.
Can you imagine what happens to your energy levels, sleep, health and moods, when your gut isn’t performing to its best?
Knowledge of the gut-brain connection has increased 10-fold over the past decade. This has been due to improved brain research as well as genetic research. Both have opened the door towards understanding gut health and the link to disease, especially the effect of the accumulation of inflammatory changes as we get older.
With menopause heralding in the transition towards our ageing, this is a critical time of life to sleep all night, restore health to our body and for those of you who need to lose weight, this will also have a positive impact on your anxiety levels and energy.
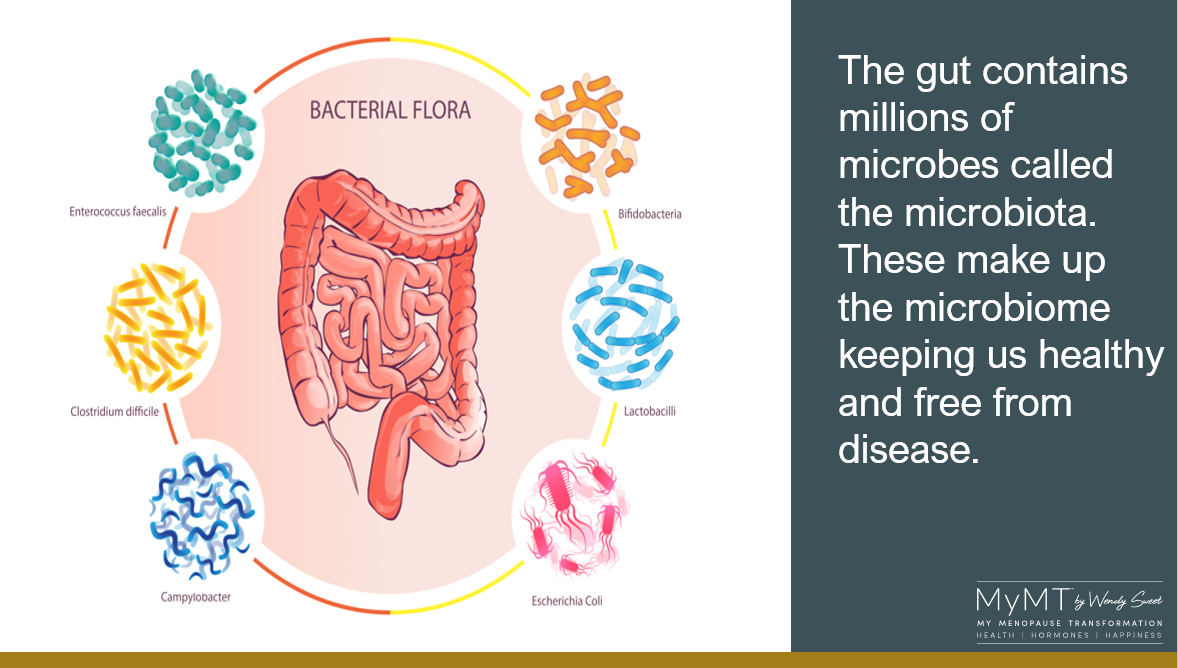
What is the gut microbiome and why does it matter to us in menopause?
The microbiome is the community of bacteria that lives in our gut and elsewhere in our body.
“The connection between the brain and gut is because messages are sent up and down the vagus nerve – the major nerve that runs from our brain to our heart, stomach and intestines. The vagus nerve therefore, has a profound influence on the gut microbiota as well as pro-inflammatory markers.
The reason for this, is because the vagus nerve transfers stress cytokines (inflammatory markers) between the gut and the brain. So, stress is the ‘hammer’ which acts on the brain and the gut. When we keep activating our stress response, then this increases the ‘leakiness’ of the gut. When the gut is leaky, we lose the ability to absorb the nutrients we need for our health and this increases oxidative stress in the body.” [Professor Zoltan Sarnyai, 2019)
I couldn’t agree more! I know from my own experience that when we aren’t sleeping one of the major changes that we experience as levels or our reproductive hormones decline, is insomnia, or interrupted sleep.
When we aren’t sleeping our gut isn’t healing properly overnight, so we accumulate pockets of inflammation throughout our digestive system.
Add to this, our changing food and chemical environment over the decades and our increasing exposure to medicines such as antibiotics, then it’s no surprise that we arrive in mid-life and we have changing gut health. But there are other changes that occur to our gut as well.
These include changes to the enzymes that break down food, changes to our gut motility (movement) and changes to our liver function (we produce less bile to break down fats). As well, for those of you who are doing lots of exercise and/or you are under a lot of stress, then your body stays in ‘fight or flight’ mode. This causes your vagus nerve to be stimulated more often. Some of you may experience frequent loose bowels which arrive during menopause. [Conversely, those of you who don’t do much exercise, may become more constipated. This is because our gut motility (movements) slow down as we go through menopause].
When all of these factors collide in mid-life, then the organ that also suffers is your lovely thyroid gland. It goes into ‘distress’ as it tries to re-balance the internal hormonal environment. As such you begin to feel your heart rate increase, then in response to this your blood pressure increases, your temperature goes up and boom – your hot flushes and anxiety levels increase as does your irritability, changing mood and of course, for many of you, your depression.

Why your Thyroid Matters:
Your thyroid gland produces hormones that are integral to the function of your gut microbiome and your brain.
If you do have a digestive disorder, such as Irritable Bowel Syndrome or Diverticulitis, then this inflammation disrupts function in the gut. In turn, your gut microbiome and therefore, disrupts your thyroid function, often speeding up your heart rate and making you feel more anxious. When your thyroid isn’t functioning as well as it should (too much or too little), this causes further disruption to your moods, motivation and emotional state (this is because your thyroid controls your heart rate, blood pressure and influences the activity of the vagus nerve).
In menopause, this can present as increased anxiety, depression and brain fog. Hence, restoring gut health and improving your gut microbiome is fundamental to improving your anxiety, brain fog, depression and even your weight.
3 Things You Can Do to Help Manage your GUT HEALTH:
When we understand the powerful connection between the brain, the gut, the vagus nerve, existing gut inflammation AND menopause, then we need to focus on these three factors:
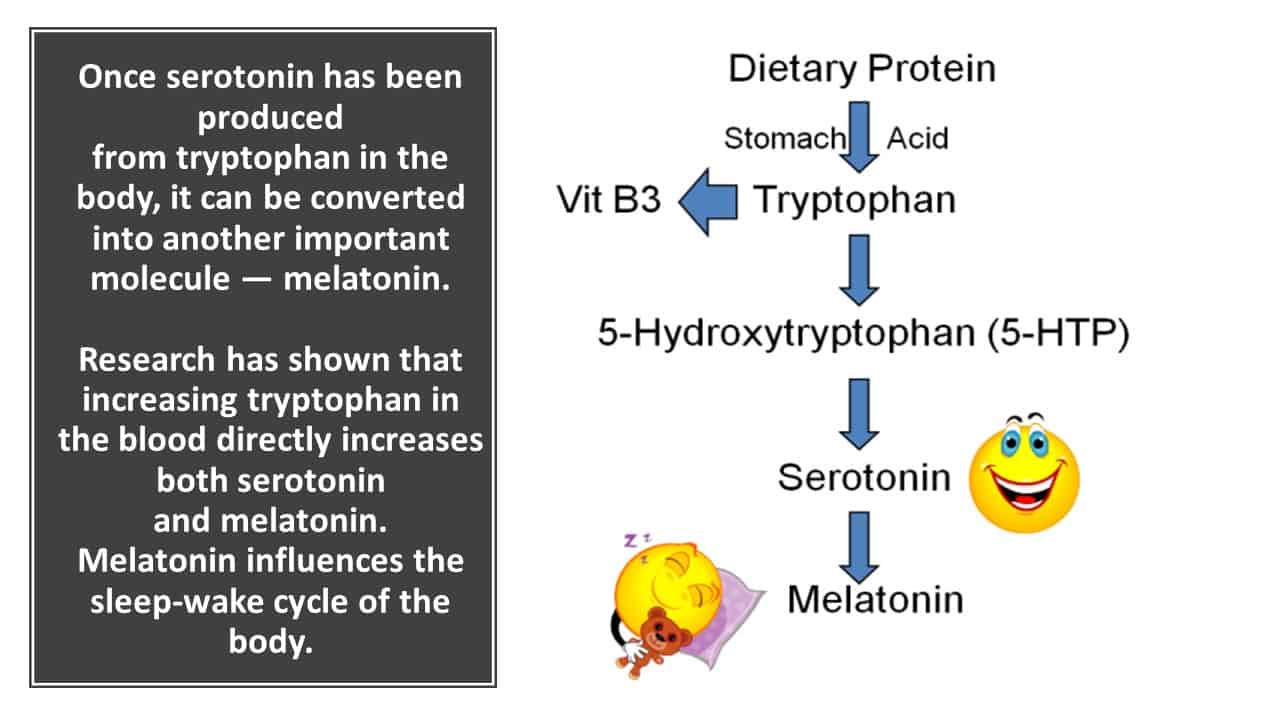
- Sleep All Night – as I keep saying to women, if you aren’t sleeping, then you aren’t healing and your heart rate stays higher during the day. This alone makes you feel more anxious because your nervous system stays ‘wired’ all day long and as a consequence of this, your gut which is serviced by the same nerves as your heart. may become irritable. As I’ve often mentioned before our gut is also on a 24 hour circadian rhythm as are all of our major organs, so we need to improve our sleep in order to improve our gut. This is why in both of the MyMT programmes, the first module you receive is called ‘SLEEP ALL NIGHT‘ – in this I teach you how to change your diet, how to sleep all night and how to turn around your hot flushes and night sweats, so you aren’t waking up! As well, if you are in anti-depressants, then there is a Gut Health module for you to listen to as well.
- Improve your Food Quality and Vegetable Diversity –
Professor Rosemary Stanton of Australia has been studying the health of the population in Australia for over four decades now. As she stated at the conference – “The way to heal the gut is to have diversity in vegetable intake and increase fibre. This is what the gut has been designed for. Decades of low fibre, processed foods have resulted in worsening health of the population and a plethora of diseases which are mainly related to our changing food environment.”

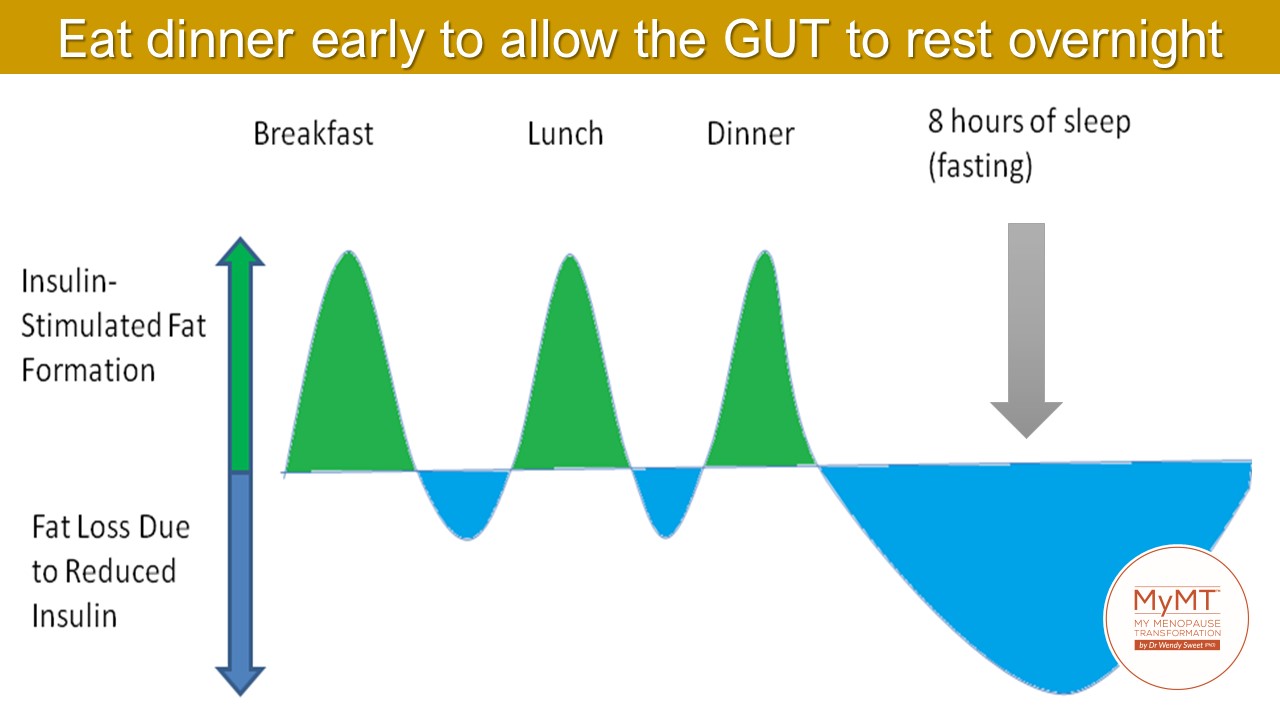
3. Allow your gut to empty fully and heal overnight. I encourage women as much as possible to allow their digestive system to rest for 12 hours overnight. This means that the timing of food and fluid is important. If we can avoid food for around 12 hours overnight (this changes obviously for shift-workers) then our digestive system gets the chance to actually digest and absorb the food that we eat during the day.
A healthy gut microbiome is a diverse microbiome, which has a large number of bacteria. When we have a healthy gut, then we also help to improve our mental and emotional health. During menopause, this includes anxiety, foggy brain and depression. It is absolutely vital that women turn around their gut health, in order to improve their mental health and overall health as they age.
In both of the MyMT programmes, I have a scientifically designed GUT REHAB programme which steps women through what to do to improve gut health. [This is now available as a stand-alone module too]. Whilst some of you may need medical intervention for improving both gut health (e.g. with probiotics specifically designed to improve certain bacteria that have been diagnostically checked as low or too high) or depression, however, underlying any of these medical interventions should also be sleep, diet and exercise strategies that help to reduce the inflammation that has typically been building up for decades.
Can I help you with your symptoms?
If you are struggling with your mid-life weight, health or symptoms, then come on board if you can into my 12 week online programmes. Programs are normally available for NZ$399 each, but please do check out the MyMT website or subscribe to our newsletter to be alerted to any promotional offers.
Or as a starting point, you can purchase my online Masterclass on Menopause. This is only NZ$15 (approx. AUS$14, US$9 or UK£7.5). During lockdown I put my live-event into an online format for you and took 50% off the usual cost of a ticket. I hope you can join me in this powerful 2 hour webinar. The great news is that now you can watch it anytime, anywhere and even pause it whenever you like and go and make yourself a cuppa too.
I hope you can join me.
Dr Wendy Sweet, (PhD), Member: Australasian Society of Lifestyle Medicine/MyMT™ Founder & Coach

References:
Albert P. R. (2015). Why is depression more prevalent in women? Journal of psychiatry & neuroscience : JPN, 40(4), 219–221.
Feraj, J. (2017). Micro-nutrients, depression and inflammation among women of reproductive age. Doctoral Dissertation 993, University of Massachusetts.
Freeman, E.W. (2015). Depression in the menopause transition: risks in the changing hormone milieu as observed in the general population. womens midlife health 1, 2. https://doi.org/10.1186/s40695-015-0002-y
Glezerman, M. (2016). Gender Medicine. Duckworth & Co Publ.
Graziottin A. & Serafini A. (2009). Depression and the menopause: why antidepressants are not enough? Menopause Int. Jun;15(2):76-81. doi: 10.1258/mi.2009.009021. PMID: 19465674.
Heitkemper, M., & Chang, L. (2009). Do fluctuations in ovarian hormones affect gastrointestinal symptoms in women with irritable bowel syndrome?. Gender medicine, 6 Suppl 2(Suppl 2), 152–167. https://doi.org/10.1016/j.genm.2009.03.004
Mulak, A., Taché, Y., & Larauche, M. (2014). Sex hormones in the modulation of irritable bowel syndrome. World journal of gastroenterology, 20(10), 2433–2448. https://doi.org/10.3748/wjg.v20.i10.2433
Nie, X., Xie, R. & Tuo, B. (2018). Effects of Estrogen on the Gastrointestinal Tract. Dig Dis Sci 63, 583–596.
Odamaki, T., Kato, K., Sugahara, H. et al. (2016). Age-related changes in gut microbiota composition from newborn to centenarian: a cross-sectional study. BMC Microbiol 16, 90. https://doi.org/10.1186/s12866-016-0708-5
https://www.researchgate.net/publication/322946988_Prevalence_of_Thyroid_Dysfunction_in_Irritable_Bowel_Syndrome
Veira, A., Castelo, P. et al, (2017). Influence of oral and gut microbiota in the health of menopausal women. Front. Microbiol.
Related Tag: Menopause Treatment

