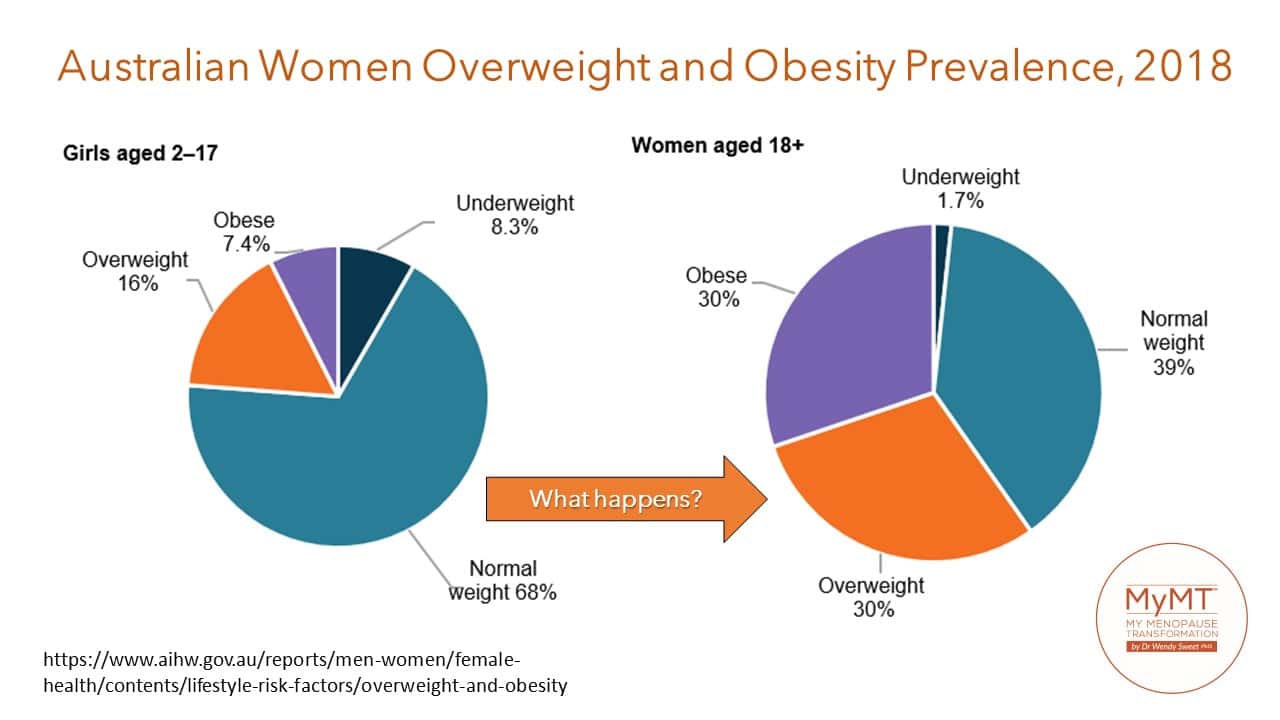
It’s amazing to think that Type 2 diabetes and obesity was rare in our parent’s generation.
But today, in many western countries, it is the fasting growing chronic condition – especially in women aged 50 – 59 years. In Australia alone, 280 Australians develop diabetes every day (Diabetes Australia). That’s one person every 5 minutes. The growth, according to researchers, is increasing at a faster rate than other chronic diseases such as heart disease and cancer.
As Practitioner’s working with midlife women, keeping up to date with research can be challenging. Overweight and obesity research is an important topic however, especially for those of you working with overweight or obese midlife female clients. Increased fatigue and menopause go hand-in-hand, and for numerous women, overweight or not, it’s as if an all consuming fatigue suddenly arrives, whether women are sleeping or not.
In 2023, a Diabetes Symposium run by the Australasian Society of Lifestyle Medicine last year, offered fascinating new insights into how insulin resistance and Type 2 diabetes management is having a (re) focus on liver, pancreatic fat and weight management.
Having immersed myself in liver-health research and the role of menopause hormonal changes on the liver and gall-bladder when my own weight reached an all-time-high during menopause, it made sense to me that both the liver and pancreas are important organs in fatigue and weight management in midlife women.
Fatty liver disease and the progression towards Type 2 Diabetes are both main contributors to mid-life women putting on belly-fat and becoming overweight and/or obese as they move into their post-menopause years.
The liver and muscles are important organs to not only utilise and store glucose and therefore, rely on the function of insulin, but they also use and store fat.
Hence, becoming aware of what happens to these organs and tissues when they become resistant to the role of insulin during menopause is important. Many of you already know about the role of insulin. This powerful hormone, secreted by the pancreas, carries glucose to the brain, liver and muscles.
With obesity and overweight status, as well as menopause hormonal changes, the glucose uptake pathway within the liver and muscles may change. Not only is this due to muscles re-modelling as oestrogen levels change, but also because the liver is re-modelling too.
When the glucose-uptake pathway becomes dysregulated, a condition called insulin-resistance may occur. It is the pre-cursor to Type 2 Diabetes because both the liver and muscles become ‘resistant’ to the normal role of insulin, which helps glucose to be carried and utilised throughout the body, but importantly, in both the liver and muscles.
If muscle and liver cells don’t uptake glucose from the blood to be used as fuel for energy, the glucose spills over into urine – many of you with clients who have Type 2 diabetes or pre-diabetes know that the urine is an important diagnostic organ in diabetes.
So too are fat cells.
If the normal uptake of glucose into liver and muscle cells becomes disrupted, and insulin-resistance occurs, then excess glucose is also carried to fat cells.
Furthermore, if liver cells are accumulating too much fat, this is also associated with insulin-resistance and weight gain. I wasn’t surprised to hear one of the speakers, Professor Rosemary Stanton, mention that fatty liver disease can appear within 2 months of Type 2 diabetes arriving.
As such, women begin to change their health status, moving from “I wasn’t overweight as a young girl” to “What the hell happened? Here I am at 50+ and overweight and being told I’m pre-diabetic?” I’ve heard this for many years from women joining me on the MyMT™ Transform Me Weight Loss program.
The health research stats in Australia are alarming. People with diabetes, are between two and four times more likely to develop heart disease – and for those of you who read my articles in my other MyMT™ newsletters, you know that this is a topic that I write about frequently.
Dr Cyrus Khambatta is a Type 1 Diabetic. He knows all about diabetes and has made it his passion to research what is going on and why. Listening to his talk, he spoke about the need to start a low-fat diet to reduce the effect of NAFLD and fat deposition within and around muscles. His research was fascinating.
“To master diabetes, you must first deal with the liver, because excess fats in the diet can cause hyper-inflammation of the liver and this in turn increases glucose spilling out into the blood (hyperglycemia).”
Every bit of research he presented (as well as others who presented later in the day), backed up my readings on women in menopause and their weight gain. And why, to reset metabolic health, overweight and obese women should go on a low-fat, vegetarian or vegan diet and increase their fibre.
This is my approach too. Which goes against much of the emphasis on a high-fat, high protein Keto diet that is readily promoted these days.
In the symposium, a number of Diabetes researchers supported the new, low-fat, higher fibre nutritional approach to managing weight gain in Type 1 and 2 Diabetes management and insulin resistance.
Dr Cyrus Khambatta, Professor Neal Barnard (George Washington School of Medicine), Professor Rosemary Stanton (University of NSW), Professor Claire Collins (University of Newcastle), Professor Gary Williamson (Monash University) and the University of Glasgow’s Professors Mike Lean and Roy Taylor, were a united voice when it came to talking about diabetes research and liver fats.
They all agreed that when it comes to both weight loss and Type 2 diabetes remission, the health of the liver matters first and foremost.
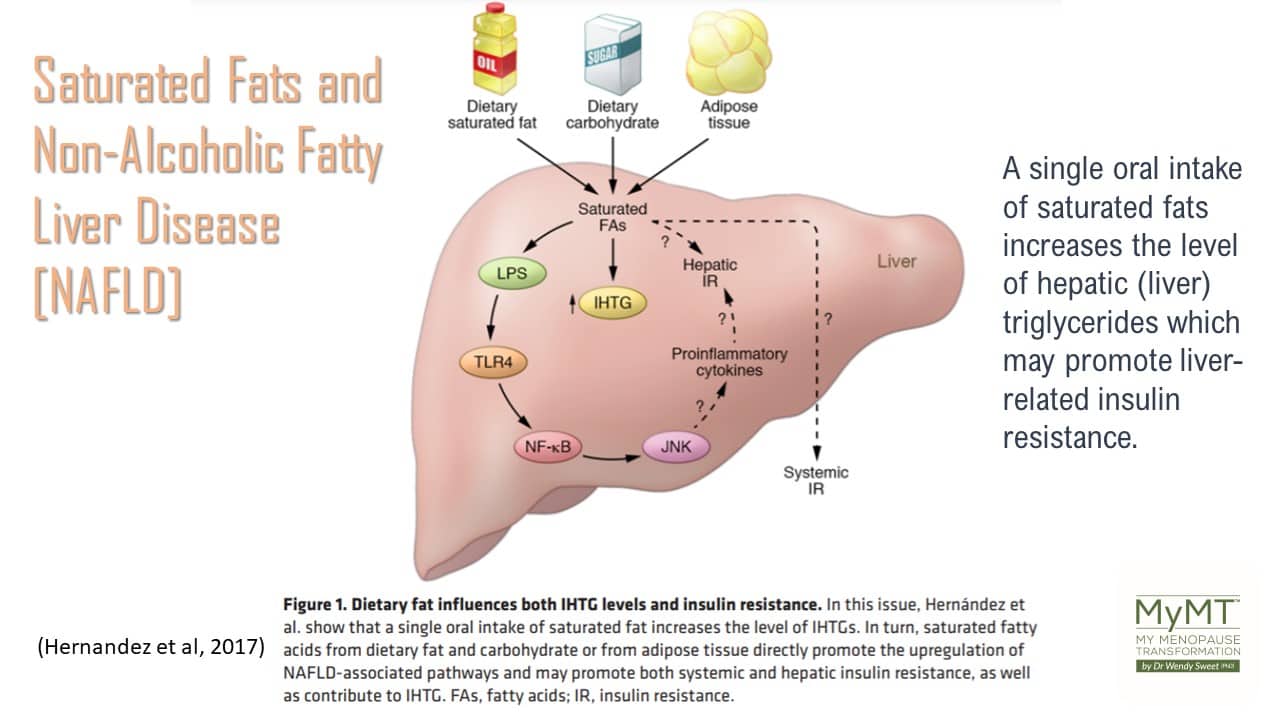
Every bit of their research matched my readings too. In order to turn around weight loss and the risk of metabolic syndrome, women need to follow a low-saturated fat diet and remove highly processed foods in order to allow the liver to reduce the storage of fats and excess glucose.
Many of you will know that an intake of highly processed foods increases blood glucose. Couple this with a diet high in saturated fats, then this combination may increase liver-clearance mechanisms, as well as gallbladder responses. This may contribute to increased liver inflammation, which for women in menopause, can be a health disaster.
Excess liver fat and inflammation can lead to insulin resistance and the slippery slope towards Type 2 diabetes.
A New Nutritional Approach to Managing Insulin Resistance:
Low fat, Low GI and Vegan (with a B12 supplement) is the new nutritional approach to managing Type 2 diabetes and losing weight in our mid-life and older years.
Increasing fibre sits alongside this advice too. Fibre is intricately connected to the health of the gut microbiome – it is ‘food for the microbiome housed in your large intestine’. Most importantly for women who are overweight and navigating menopause and post-menopause, fibre helps to slow down the rate of glucose absorption into the bloodstream, which is great news for helping to manage insulin resistance.
It is well known that excess body weight and insulin resistance may lead to Type 2 diabetes and other major health problems.
But as Diabetes researcher, Associate Professor Neal Barnard from Washington State University mentions, obesity tends to be uncommon in individuals whose diets are based on plant-derived foods. In clinical trials, two explanations have been offered.
- A high-fibre, low-fat diet has low energy density, which reduces energy intake.
- A low-fat, vegan diet increases the thermic effect of food. This is the increase in metabolism that occurs in the body which contributes to total energy expenditure.
Perhaps the strongest evidence comes from the fact that when a plant-based diet is consumed, the liver and muscles have reduced fat storage capacity.
With a vegan diet, intramyocellular lipids (fats stored in droplets in muscle cells) are lower, suggesting that when both muscle and liver fats are lower, the body burns more energy through increased mitochondrial activity and post-prandial (after-eating) metabolism. (Kahleova, Petersen & Barnard, 2021).
This is particularly important, because the accumulation of excess fats in muscle and liver cells may also be associated with insulin resistance and Type 2 diabetes.
My own weight soared as I moved through my early 50s. I had no idea why this was at the time, because I was doing vigorous exercise and eating a high-fat and high-protein, diet which was promoted to me at the time. But the weight wasn’t shifting. In fact, I felt heavy, bloated and unhappy with the fact that I couldn’t exercise the way I used to.
What I wasn’t doing however, was following the scientific evidence for women in menopause and how, when women are overweight or obese at this life-stage, there are numerous changes going on in organs, including both the liver and muscles.
Women in their 50s today are a generation of women who have been forgotten in the mid-life lifestyle-change research and my passion is to change this, hence I have all this information and more in the MyMT™ Menopause Weight Loss Coach Course. I hope you can take your learning to another level on this powerful CPD course sometime.
Whilst there is a primary emphasis on ‘just’ hormonal treatments in menopause, the research suggests that weight gain in menopause requires a different approach because there is so much more to ‘Women-opause and weight gain’ than we think.
Dr Wendy Sweet (PhD)/ MyMT™ Founder & Member: Australasian Society of Lifestyle Medicine.

References:
Australian Institue of Health and Welfare: https://www.aihw.gov.au/reports/diabetes/diabetes/contents/how-many-australians-have-diabetes
Brady CW. (2015). Liver disease in menopause. World J Gastroenterol. Jul 7;21(25):7613-20. doi: 10.3748/wjg.v21.i25.7613. PMID: 26167064; PMCID: PMC4491951.
Kahleova H, Petersen KF, Shulman GI, Alwarith J, Rembert E, Tura A, Hill M, Holubkov R, Barnard ND. (2021). Effect of a Low-Fat Vegan Diet on Body Weight, Insulin Sensitivity, Postprandial Metabolism, and Intramyocellular and Hepatocellular Lipid Levels in Overweight Adults: A Randomized Clinical Trial. JAMA Netw Open. Nov 2;3(11):e2025454.
Khambatta, C. (Podcast). https://www.pcrm.org/news/exam-room-podcast/fat-fruit-sugar-and-diabetes-cyrus-khambatta-phd
Ma Y, Hébert JR, Li W, Bertone-Johnson ER, Olendzki B, Pagoto SL, Tinker L, Rosal MC, Ockene IS, Ockene JK, Griffith JA, Liu S. Association between dietary fiber and markers of systemic inflammation in the Women’s Health Initiative Observational Study. Nutrition. 2008 Oct;24(10):941-9.
Montiel-Rojas D, Nilsson A, Santoro A, Franceschi C, Bazzocchi A, Battista G, de Groot LCPGM, Feskens EJM, Berendsen A, Pietruszka B, Januszko O, Fairweather-Tait S, Jennings A, Nicoletti C, Kadi F. Dietary Fibre May Mitigate Sarcopenia Risk: Findings from the NU-AGE Cohort of Older European Adults. Nutrients. 2020 Apr 13;12(4):1075.
Ramin S, Mysz MA, Meyer K, Capistrant B, Lazovich D, Prizment A. A prospective analysis of dietary fiber intake and mental health quality of life in the Iowa Women’s Health Study. Maturitas. 2020 Jan;131:1-7.
Venetsanaki V, Polyzos SA. (2019). Menopause and Non-Alcoholic Fatty Liver Disease: A Review Focusing on Therapeutic Perspectives. Curr Vasc Pharmacol. 17(6):546-555. doi: 10.2174/1570161116666180711121949. PMID: 29992886.


