There she was lying in the snow. We thought that she had broken a bone, but fortunately she hadn’t. As she picked herself up and caught her breath, it got us talking about bone health in mid-life and how, the thought of breaking a bone and falling puts us off doing the adventurous activities that we’ve enjoyed doing for decades.
Now that I’m in post-menopause, I think about my ageing bones more than ever. Especially since I had a recent bone scan which showed a decline in my bone health – yes, despite all the exercise that I do and have done for years. But some of this exercise wasn’t suited to the evidence for the right amount, type and intensity of exercise for our ageing bones. Hence, this article just for you. Whether you’ve had your bones checked or not, it’s an important topic to understand as we move through menopause.
It was no surprise to me that for this year’s theme on World Menopause Day 2021, the International Menopause Society (IMS) chose women’s bone health as their theme. They have even released a brand new White Paper on this important topic. As the paper states, ‘Osteoporosis and associated fractures are the most common metabolic bone disease and represent a major global health problem, contributing to 8.9 million fractures worldwide on an annual basis.’
We can all expect some deterioration in our bone health as we age. That much is clear. In fact, the research states that there is a loss of 1-2% from the age of 60 years, with 1.5% per year from the spine and up to 1.4% in the femoral neck of the femur (Benedetti et al, 2018).
This is why bone health is an important topic for all of us – myself included. And it’s why, I want to focus you on the right amount and type of exercise that you can do to allay the progression of deteriorating bones as you age based on relatively new research about the effectiveness of physical exercise on bone density. (Benedetti et al, 2018).

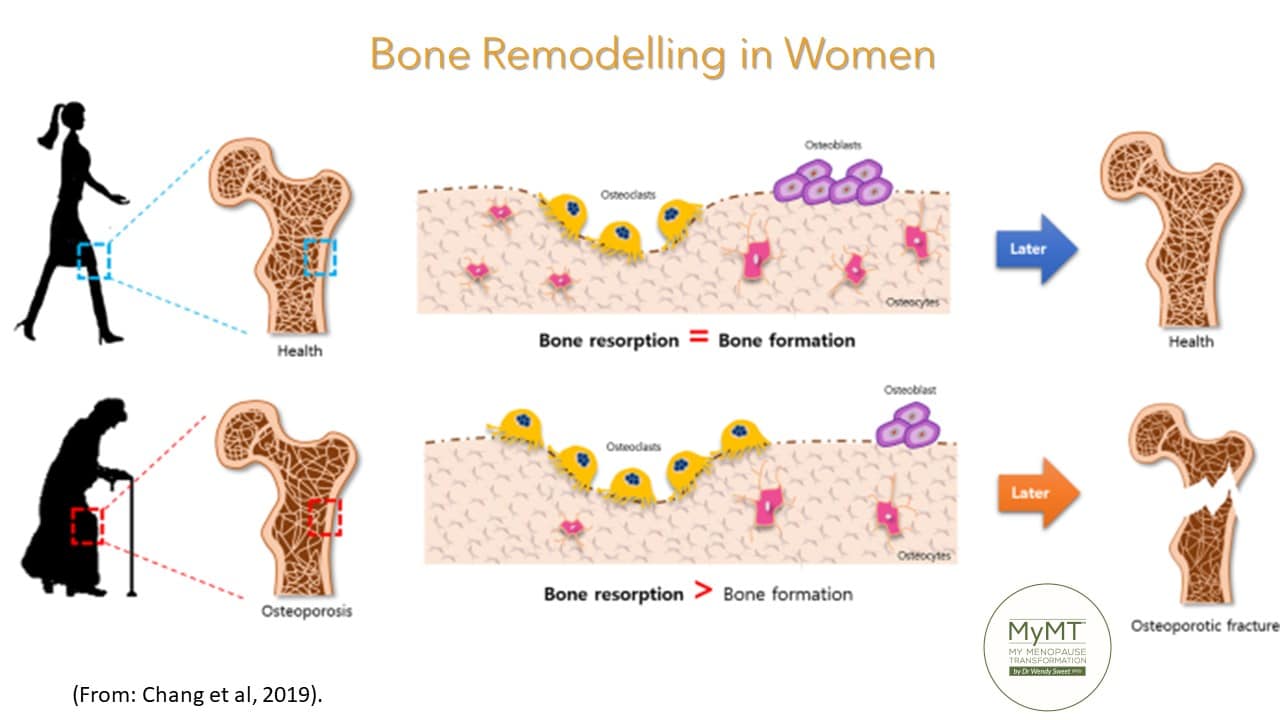
In the early 1990s, osteoporosis was defined as a systemic skeletal disease characterised by low bone mass and deterioration in the micro-architecture which results in an increase in bone fragility and increased susceptibility to fracture. This definition underpinned the pivotal concepts of fracture and bone mineral density (BMD).
Today, estimations of BMD have become a reality with the advent of the DEXA scanner. Results from these scans offer women a fracture risk probability over time. Maybe you’ve had one of these scans as I did recently and want to focus on not only preventing fracture risk, but also preventing any further deterioration over time?
If so, then we must consider exercise in this approach, especially in post-menopause. Relatively new research on the effect of physical exercise on bone density in women who already have osteoporotic changes (which is possibly most of us in post-menopause!), is clear on the amount, type and intensity of exercise we need to do to boost our bone health as we age, so here it is for you.
- Exercise to improve bone density is SITE-SPECIFIC. For example, if your bone loss is in your vertebrae, then you need to strengthen your back muscles and do specific spinal exercises, which don’t lead to wear and tear. Same with your arms and legs. It’s interesting that a DEXA scan only does hip and lumbar spine estimations. It doesn’t do the arm bones, nor the cervical or thoracic spine, so we also need to include exercises that specifically target these areas in our exercise routines as well.

2. Aerobic exercise helps to improve enzymatic activation of the osteoblasts (these are the bone forming cells). Walking is more effective than cycling as are other weight-bearing activities to prevent further loss.
3. Muscle strengthening of the upper extremities and spinal muscles are important for bone density of the vertebral column.
4. Higher load and lower reps is the most effective exercise prescription. The effectiveness specifically for bone density is related to LOAD (70-90% of maximal effort) for only 8-10 REPETITIONS of 2-3 SETS. (I describe these in my Rebuild My Fitness module on bone health).
5. Progression from RESISTANCE BANDS to WEIGHTS is effective for those women who are beginners. I have these types of workout programmes in my Rebuild My Fitness programme designed for women wanting to renew their physical activity levels again.
6. Bone-loading exercises must be performed for a YEAR or MORE to see changes. At least 2 times a week for specific bone-strengthening exercises.
7. Upper back exercises are significantly important. Muscles pull on bones and therefore, it is this action that stimulates bones to turnover new cells. Anti-gravitational extension in the prone position with a loaded backpack was specifically mentioned in the research to prevent vertebral (spinal) fractures.
8. Multi-component training of numerous muscle groups is important. A combination of different exercises including aerobics, resistance training, balance activities and dancing!) have all been evidenced to help with bone density.
9. HIIT cardio showed little change in bone density in older women.
10. Training with Vibrating Platforms has emerging evidence only. This type of vibration platform training is indicating relatively good evidence for stimulating the muscle receptors to stimulate the bones to turn-over cells.

But it’s not just about osteoporosis or osteopenia (the first phase of osteoporosis). There is another condition which hits us in menopause due to our changing reproductive hormones. This condition is the muscle-loss condition called SARCOPENIA.
low levels of oestrogen and changing testosterone levels too, cause muscles to lose volume and size. But here’s the thing, body fat does not protect against osteoporosis development either.
This is why strengthening our muscles is just as important for us as strengthening our bones. If our muscle density is reducing and our fat levels are increasing, not only do we become weaker, but there is less stress being placed on your bones from the movement of muscle, tendons and ligaments pulling on the ends of your bones. (If your joints are sore, then I cover what to do to turn this around in my RESTORE YOUR JOYFUL JOINT Module.
Pulling and pushing actions affect bone cell turn-over too. The ends of your bones (the epiphysis) are where you get NEW BONE CELLS forming and the epiphysis responds to pushing and pulling activities. These activites help to re-model the bone which then requires critical bone-building nutrients, such as Vitamin D, calcium, magnesium and phosphorous, to help healthy, new bone cells to be formed.
But here’s the thing – hormonal changes in menopause, and other factors such as gut and liver inflammation can INHIBIT the uptake of these vital nutrients into our bones. Hence, other factors impact on bone disease risk too. These include:
1. Decreased physical activity as you age.
2. Decreased amino-acid (protein) intake and uptake due to changing LIVER inflammation. I talk a lot about the liver Proteins are ‘turned-over’ in your liver and if you aren’t getting adequate healthy proteins into your diet, then this can have a down-stream effect on sarcopenia too.
3. Loss of activation of the motor-units (nerves) which stimulate muscles to contract. Muscle movement is controlled by your nervous and hormonal system and when we activate all of our muscles, then this is great for bone and muscle strength. It’s where the old term ‘use it, or lose it’ comes from. When your muscles are stimulated to pull on bones, then your bones are also stimulated to turn-over new bone cells.
4. Age-related decline in the hormones which assist your bones to stay strong. These hormones include testosterone, growth hormone, Vitamin D .
5. Internal Inflammation. For example, gut inflammation can inhibit the uptake of key nutrients that support bone health as does not sleeping well overnight. If you aren’t sleeping, your body isn’t healing and repairing itself.

6. The wrong DIET for menopause. A typical Western diet that is high in processed foods, sugar and alcohol is typically not osteopenia or osteoporosis friendly. This is why I say when it comes to menopause and the risk of oesteoporosis with age, we all need to improve our diet to better meet our changing hormonal environment which will become our ‘new-normal’ the older we get.
7. Being too thin and small in stature. If you have a thin bone structure, and weigh UNDER 60 kg, then you are at greater risk for osteoporosis as you get older. Your goal therefore is to increase your muscle mass and maintain a body weight that decreases your risk as you age.
Do you know what your RISK for osteoporosis is? If you don’t, then go and get your bone density tested. If you are concerned about your changing bone strength and density, then make sure you talk to your health or medical professional so you can get this tested. Clinically the ‘gold-standard’ for measuring bone density is a Dual Energy X-Ray Absorptiometry or DEXA scan and is available through your health provider.
But whether you are at risk or not, then I also encourage you to visit the website and look at the MyMT™ Re-Build My Fitness programme. I am so passionate about getting women back into healthy exercise as they age, that I have designed this programme with this purpose in mind. The programmes can be down-loaded and I have webinars and videos to explain the exercises to you.
Even if you go to the gym, there are programmes that suit your needs either at home or with gym-based equipment. I’ve designed everything you need for your EXERCISE NEEDS as you age. The programmes are progressive and designed for both beginners and intermediate level women to build their stamina through walking or other cardiovascular exercise, build their strength, flexibility, balance and help to stabilise the core muscles which support posture and stability. All factors which influence health and wellbeing as we age!

References:
Benedetti, M., Furlini, G. et al. (2018). The Effectiveness of Physical Exercise on Bone Density in Osteoporotic Patients. BioMed Research International, (4), 1-10
de Villiersa, T. & Goldsteinb, S. (2021). Update on bone health: the International Menopause Society White Paper 2021. Downloaded from: https://www.imsociety.org/education/world-menopause-day/#whitepaper
Kruger, M. & Wolber, F. [2016]. Oesteoporosis: Modern paradigms for last centuries bones. Nutrients (8),376, 1-12.
Lohana, C. & Samir, N. (2016). Risk Management of Osteoporosis in Postmenopausal Women. Global Journal of Health Science, Vol. 8, No. 11; 36-44.
Osteoporosis NZ, www.osteoporosis.org.nz
Santos, Lívia et al. (2017). “Exercise and bone health across the lifespan.” Biogerontology vol. 18,6: 931-946. doi:10.1007/s10522-017-9732-6
Sözen, T., Özışık, L., & Başaran, N. Ç. (2017). An overview and management of osteoporosis. European journal of rheumatology, 4(1), 46–56. https://doi.org/10.5152/eurjrheum.2016.048


