“When my mum was in her 50’s she gave up working. I can’t do that though. I need to keep working as long as I can. It is quite tiring and stressful though, then menopause on top of that, makes it tough. But nobody talks about it at work, though we are all probably thinking about it.” [Jane, Study Participant].
The conference room was packed to over-flowing. One savvy company in New Plymouth, New Zealand, bought my ‘Masterclass on Menopause’ seminar to the workplace this week. “I had no idea it would be such a popular topic” said the surprised HR Manager. I wasn’t surprised at all.
What is more surprising to me, is that the topic has been left out of workplace-wellness education for so long. Since the 1950’s in New Zealand, approximately 60 percent of all those aged 15 and older have been employed. Yet, in a 2014 paper prepared for the the National Advisory Council on the Employment of Women (Calister, 2015*), within this period the long term trend has been increasing employment rates for women and decreasing employment rates for men. I know from my own doctoral studies that Baby-boomer research is replete with the knowledge that for both women and men, that whilst there has been a shift to earlier retirement from the mid 1950’s through to the mid 1980’s, since then, there has been a significant reversal of this trend. Hence, more women than ever before are now working into their 50’s, but in a similar vein to the exercise and health education industries, peri-menopause and menopause, has been mainly invisible in workplace health and wellness programmes.
This is why I was so excited to share the topic that fuels my passion these days, and talk to a group of mid-life women in a large company in beautiful Taranaki this week. The mountain was looking stunning too.
 My own doctoral research on women’s healthy ageing, revealed that women are finding it tough to understand all the changes that they are experiencing in their mid-life hormonal transition, and more importantly, how to manage the symptoms that arrive at this time of life too. Many of my middle-aged (50-62 years) study participants (all of whom remained in the workforce) were turning to fitness pursuits thinking that ‘more is better’. Little did many realise that this ‘go hard or go home’ mantra, when intersecting with peri-menopause and a lowering oestrogen environment, was also a cocktail for sore muscles and joints as well as poor sleep in their menopause transition.
My own doctoral research on women’s healthy ageing, revealed that women are finding it tough to understand all the changes that they are experiencing in their mid-life hormonal transition, and more importantly, how to manage the symptoms that arrive at this time of life too. Many of my middle-aged (50-62 years) study participants (all of whom remained in the workforce) were turning to fitness pursuits thinking that ‘more is better’. Little did many realise that this ‘go hard or go home’ mantra, when intersecting with peri-menopause and a lowering oestrogen environment, was also a cocktail for sore muscles and joints as well as poor sleep in their menopause transition.
As I explained to women attending my seminar, when our sleep changes, this has a down-stream effect on our thyroid and adrenal health. Which means that our hot flushes increase in frequency and severity and if this is coupled with heavy exercise or nutrition that is not set up for the right type or timing of nutrients to help manage our hot flushes and energy levels, then the inflammation builds up not only in our joints and muscles, but in our gut and liver as well. All together, the accumulation of symptoms when put up against increasing workplace stress or increased daily physical workload as many farming women and nurses have to endure, then this can lead to fatigued and over-worked adrenal glands. When the adrenals are over-worked then we stay in ‘fight or flight’ mode for longer, and this causes increased feelings of anxiety, heart palpitations, frustration and a drop in energy levels, especially in the afternoon. And when you work in a job that requires you to be firing on all cylinders and making all sorts of decisions, especially for those women who have leadership roles, this can all lead to a turn for the worse, not only for women’s physical health during their menopause transition, but also for their emotional health as well. As Gavin Jack and other researchers from Australia contend in their extensive studies on menopause in the workplace –
“the many specific and interconnected health, lifestyle, ageing and work-related concerns of women aged 45 years plus (including menopause) can influence women’s participation in paid employment and engagement and performance whilst at work and these are often overlooked.” (Jack et al., 2016)*
I know from my own experience that for many women approaching their 50’s, menopause has been a topic that hasn’t really been discussed openly and certainly not in the context of health and wellness at work. This is because traditionally, menopause has been the domain of the medical and pharmaceutical industries. Which positions menopause in sickness not wellness, making the topic a reluctant one for women to discuss. I found that too. But as the last of the Baby-boomer generation enter their 50’s, many are searching beyond the promise of pills and supplements for menopause relief. When my own symptoms over-whelmed me and I didn’t find the relief I sought from pills and potions, I began to research menopause. Menopause usually occurs in women between the ages of 45 and 55 years and may result in a variety of symptoms lasting from four to eight years. For decades menopause has been managed with hormone therapies, however, my studies pointed me in the direction of wellness. I learnt that menopause symptoms can be managed holistically by changing aspects of our daily lifestyle (including nutrition and exercise) so that we work with our changing hormonal environment which is heralding in the end of our reproductive capacity. When we use specific strategies to allow our body to adapt to this ‘new-normal’ (which is what the MyMT programmes teach you), then the symptoms of poor sleep, hot flushes, night sweats, palpitations and weight gain can be resolved. However, there is a caveat to this – for working women, when workplace stress accumulates with other sources of stress (e.g. personal stress, poor diet, too much or not enough exercise) and these are present on a daily basis, menopause symptoms can stay around for years.
Workplace stress and peri-menopause do not co-exist! They compete!
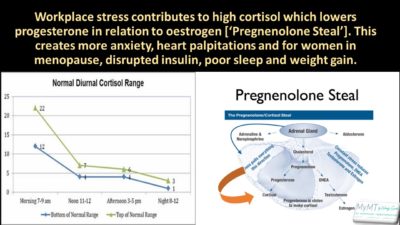
When women feel stressed, time-poor and have increasingly challenging roles to juggle between work and home environments, then our chronic stress hormone called cortisol increases over the course of the day. But this is the opposite to what should occur – cortisol should be high in the morning (it switches off melatonin, which is your sleep hormone) and then low in the afternoon and evening (to allow melatonin to rise again in a 24 hour circadian cycle). Feeling stressed at work increases cortisol (as does not eating properly) and with this, comes the ‘stealing’ of progesterone to keep making cortisol. The result? Low progesterone in relation to oestrogen which increases feelings of even more anxiety and frustration and can lead to high blood pressure, high resting heart rate, breathlessness, insomnia and for many women, increasing weight gain and sore muscles and joints. It’s what I explained in my workplace seminar earlier this week and the girls’ were fascinated. It all made so much sense and there was lots of nodding of heads.
 According to menopause and workplace research, a broad range of factors are known to influence the ability of older workers to remain in the workforce. These include:
According to menopause and workplace research, a broad range of factors are known to influence the ability of older workers to remain in the workforce. These include:
- health status
- financial position
- conditions of work including labour demand
- the availability of suitable (part-time/flexible) work that matches skills
- the presence/absence of discrimination
- the centrality of the role of work, and gender.
In a recent US survey, nearly half the working women aged 45 to 60 years found that managing menopausal symptoms in their work life was extremely or somewhat difficult. As Jack, et al. (2016) remind us, large numbers of women transition through menopause whilst in paid employment and symptoms associated with menopause may cause difficulties for working women, especially if untreated, yet employers are practically silent on this potentially costly issue. Though several papers established that vasomotor or hot flush (and associated) symptoms, have a negative impact on women’s productivity and capacity to work, this is not a uniform finding. Psychological and other somatic (body) symptoms associated with menopause can have a relatively greater negative influence. These include palpitations, high blood pressure, feelings of increased anxiety, forgetfulness and of course, mood swings.
So, what can employers do to help address these issues for our lovely menopausal employees?
Well, firstly, to me, it’s all about acknowledging that this is a normal life stage that women go through. When we do this, and with the knowledge that there are so many women at this life stage still in the workforce, then let’s get it out in the open and position peri-menopause and menopause as a topic well worth putting on the wellness agenda.
Secondly, there are practical strategies that employers should also consider and many of these are from studies that focus on the workplace environment. Strategies researched by Jack et al. (2016) as well as include:
- Ensuring that the workplace temperature and workplace design is conducive to women experiencing hot flushes. This includes having fans and/or fresh air circulating in the workplace.
- Managing psycho-social workplace factors, e.g. work stress, perceptions of control/ autonomy so that work stress does not exacerbate symptoms.
- Risk assessments to make any adjustments to the physical and psycho-social environment, such as having access to cold water.
- Provision of information and support.
- Appropriate training for front-line managers.
Whilst menopause may cause no significant problems for some working women, for others it can present considerable difficulties in both their personal and working lives. I found this out the hard-way too – and the number of women coming through my 12 week programmes will attest to that, I’m sure! During the menopausal transition women report that fatigue and difficulties with memory and concentration can have a negative impact on their working lives, but I would add that the thing that has the most impact on daily health, energy and motivation, is lack of sleep. Furthermore, hot flushes can be a source of embarrassment and distress. Many studies reports that women consider that all of these symptoms can impact on their work performance.
This is why I loved going to New Plymouth and I wish I could name the company, but they are paving the way to show that women employees in their mid-life menopause transition are valued when it comes to workplace well-being. The only thing that might be missing from their wellness agenda now, is the lovely topic of ‘man-opause‘ when men go into a low testosterone and growth hormone hormonal environment. In fact as men get older, their oestrogen levels are increasing whilst ours are declining. I love telling seminar attendees that one! And it means on both sides of the gender gap in the workplace, there needs to be understanding and empathy on both sides.
 Dr Wendy Sweet [RN/PhD] – Women’s Healthy Ageing Researcher and MyMT Creator & Coach.
Dr Wendy Sweet [RN/PhD] – Women’s Healthy Ageing Researcher and MyMT Creator & Coach.
References:
Calister, P. (2014). The employment of older New Zealand women. A paper prepared for the National Advisory Council on the Employment of Women, Ministry of Women’s Affairs, Wellington, New Zealand.
Jack, G., Riach, K., Bariola, E., Pitts, M., Schapper, J. & Sarrel, P. (2016). Menopause in the workplace: What employers should be doing. Maturitas, 85, 88-95.


