MyMT™ Education: Muscle Changes in Menopause – why heavy weight training is not for everyone.
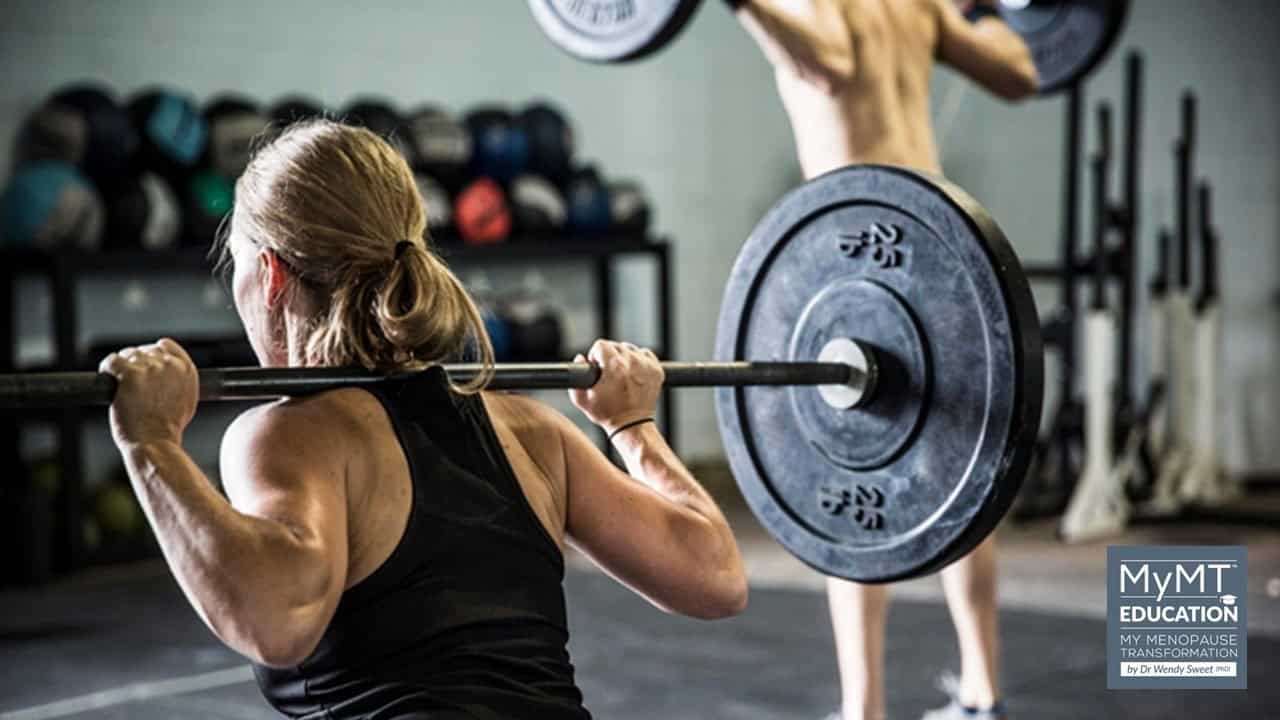
“Since my body-building competition, I’ve been trying to grow muscle, but all I’ve gained is 6kg of mainly fat. My liver had become very unhealthy”. [Lyn, Australia] What your clients do each day of their life and how they live their life affects symptoms in menopause. I’m often telling my own clients this, including former […]
Walk away menopausal anxiety, stress and sore joints.

When both Lyndie and Susi (in the photos above) came into my menopause transformation programmes, they were hardly walking anywhere. However, they both experienced fatigue, sore joints, lack of motivation and for Lyndie, her breast cancer treatments left her exhausted. They were also confused about what type of exercise was best for them. But as […]
MyMT™ Education: Menopause Depression and Exercise – A time for change.

The day I left my Doctor’s clinic with my first ever prescription for anti-depressants, was the day I pulled out all the research I could find relating to menopause-related depression, including the role of exercise. I was confused as to why, when I have never had depression in my life, it had arrived during my […]
New Research: Morning Exercise, Blood Pressure Reduction and Weight Loss in Midlife Women

In sport and exercise science, the timing of exercise remains a controversial topic. As new research (Arciero et al, 2022) suggests, some investigators favour morning exercise to enhance muscle adaptations and fuel utilization whereas, others have shown afternoon/evening exercise is most favorable to improve muscle function. As a sport and exercise lecturer for years, I’ve […]
Your Changing Muscles in Menopause: Exercise to energise, not exhaust you.

You’re not sleeping well, your gut health is playing up, your blood sugar is crashing frequently based on your monitoring and your hot flushes are through the roof. But still, you head to the gym and lift heavy weights … because that’s what you’ve done for years. That was Lyn. “Menopause changes your muscles and […]
Muscle Mitochondria: The cause of the surprising changes to your energy during menopause.

Mountains feature a lot in the lives of many MyMT™ women. They feature a lot in my family’s life too. Whether hiking or skiing, we enjoy being in the mountains, as many women on my programmes do as well. But it wasn’t always that way. One of the challenges that beset many of us as we transition […]
Fight the Fatigue: Why physical activity matters to your energy levels during menopause.

My coaching community is full of women enjoying being active again. I say ‘again’ for a reason – so many of them tell me that they have enjoyed activity all their life,but when peri-menopause arrived, aching muscles, insomnia and sore joints, left them unable to do the exercise that they used to do. They are […]
Good Vibrations: Defusing the osteoporosis time-bomb in menopause with the right exercise.

There she was lying in the snow. We thought that she had broken a bone, but fortunately she hadn’t. As she picked herself up and caught her breath, it got us talking about bone health in mid-life and how, the thought of breaking a bone and falling puts us off doing the adventurous activities that […]
‘More than just a headache’: The impact of Yoga on migraines in menopause.

Migraine is three times more common in women than in men and is the 4th leading cause of disability in women. Onset of migraine increases at menarche, with peaks in prevalence in the late 30s, and a rapid decline after menopause. While the prevalence is highest among women of childbearing age the frequency of headache […]

