This week saw me visit a progressive workplace here in New Zealand, which put menopause and lifestyle solutions on the wellness agenda. The room was full of women and men, young and old.
I’m sure that many of them were surprised as I began to talk about both gut health and heart health. But I did this for a reason … many women don’t understand that we need to take an integrated, all-over approach to the reproductive changes that our menopause transition is heralding in. There is so much focus on ovarian function and ‘just’ taking HRT, however, there is a lot happening throughout the body and looking after our gut and heart health is critical to menopause symptom management too.
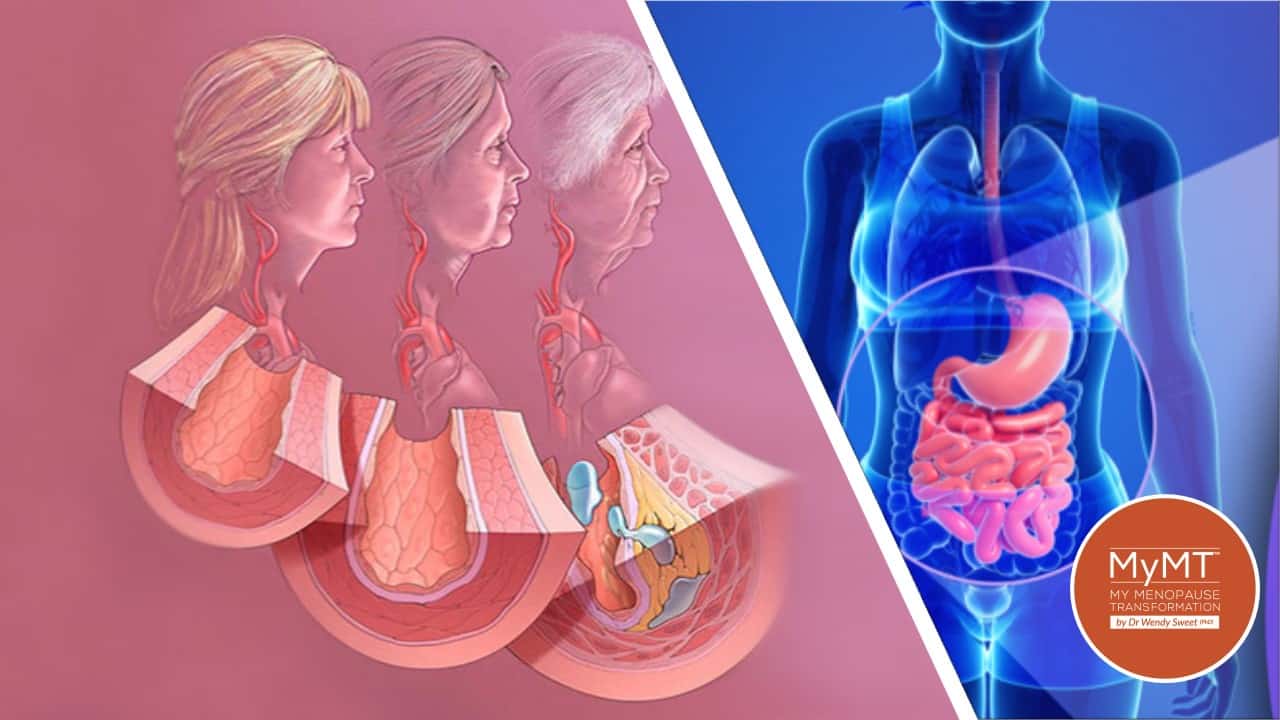
One of the topics I introduced the staff to was a condition called Vascular or Arterial Stiffness. This is now a recognised phenomenon in women’s heart health and ageing. According to Dr Angela Maas, world-renowned women’s cardiac specialist, the changes to our blood vessels begin during the menopause transition.
Un-raveling the lifestyle science specific to our menopause transition, took me hundreds of hours of study. Like so many women, I was taking endless supplements as well as HRT, but these weren’t necessarily getting to the heart of the problem – literally!
For example, I didn’t know about the connection between changing gut health in menopause, poor sleep and changing heart health, including blood pressure.
We all know that getting a good night’s sleep is crucial to our longer term health, but emerging research also suggests that when it comes to our sleep, blood pressure management and our menopause symptoms, there’s something else as well – the link between our gut health and a condition called vascular or arterial stiffness.
I spoke about this in my presentation this week and I also talk about it in my online Masterclass on Menopause. When I take these live events, numerous women say, “This makes so much sense to me now as to why I’m feeling the way I’m feeling!”
I hear from so many women who don’t understand that their irritable bowel symptoms, aching muscles, aching joints and hot flushes, are not just due to declining levels of oestrogen, but also to not sleeping and our changing blood vessels during menopause.
Changes to the Gut Microbiome Occur During Menopause
The gut microbiome has been implicated in a variety of potential
disease mechanisms including oxidative stress and inflammation that could influence vascular (blood vessel) disease. Researchers from Kings College, London, have discovered that gut microbiome diversity is linked to arterial stiffness in women as they transition menopause. [Menni et al, 2018].

Irritable Bowel Syndrome (IBS) is now known to be a disorder of gut-brain interaction and it is more prevalent in women transitioning through menopause.
IBS is characterised by abdominal discomfort such as bloating and pain, and changes in bowel function, including diarrhoea, constipation or both. It’s a disorder that needs to be diagnosed by a Specialist.
The curious thing about IBS is that it is most prevalent in women, and is known to fluctuate in terms of severity with the menstrual cycle and these effects continue through the menopause transition into the post-menopausal period of our lives.
Yes, declining oestrogen levels during menopause are contributing factors. Oestrogen decline impacts the ‘leakiness’ of the junctions in your gut wall, as well as changing the levels of your microbes in your gut, (collectively called the microbiome).
But other factors impact IBS as well, and these include insomnia, stress, diet, excessive exercise and of course, pelvic surgery. (Yang et al, 2021).
However, what we have to remember is that changes to gut health are now known to impact the hardness of your arteries – arterial stiffness – a known phenomenon for women in menopause and post-menopause.
The starting point to turn this chaos around is to change your nutrition and get good restorative sleep between 2-4am. As I mentioned to women attending my presentation this week, this is the time of night that our pituitary gland releases a pulse of growth hormone that stimulates tissue growth and gut repair.
That’s why, when we are lying awake between 2 and 4am, this release of growth hormone does not reach the threshold it needs to for healing and repairing our body, including healing our gut overnight.
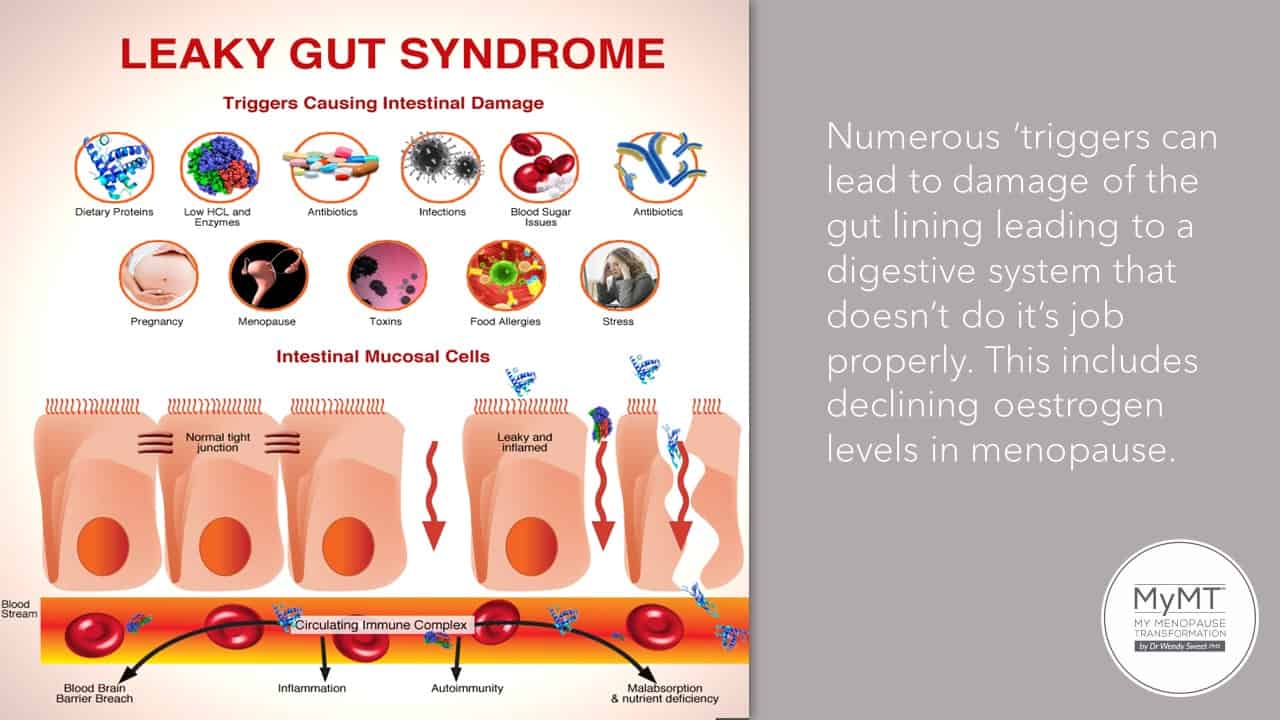
We can also change our food to help reduce gut problems and reduce the effect of arterial stiffening during menopause …
One of the most abundant proteins in your blood is called glutamine. The role it plays in helping your gut wall to maintain its integrity is as important as the role of sleep on your immune system. It is well known that many of those supplements you might be taking for your gut disorder generally have glutamine in them.
Your gastrointestinal epithelium is the lining that covers the inside of your intestine. This epithelial covering plays an important role in your symptom management as well as in your health as you age.
It impacts digestion, absorption and secretion serving as a barrier to diffusion of toxins, allergens and pathogens from the intestinal contents in the surrounding tissues.
Any disruption to this barrier causes noxious substances to enter, causing mucosal inflammation and tissue injury. In fact, with the phenomenal growth in gut health research over the past decade, it is well known that gastrointestinal diseases such as inflammatory bowel disease, irritable bowel syndrome (IBS), coeliac disease and colitis are a result of the loss of the tight junction integrity in the epithelial lining of the intestine.
As such, there is increased intestinal permeability of toxins across this usually, tight barrier.
The good news is that more recent research suggests that certain nutrients help to preserve this gut-barrier integrity, and are therefore, beneficial in the treatment of various gut health disorders. When you sort out your gut health, then this also helps to improve your sleep duration and quality.
One of these nutrients is called glutamine or you may have heard of it as L-glutamine. The terms glutamine and L-glutamine are often used interchangeably in most of the information you will come across in regard to sports and exercise performance. The difference between the two lies within the chemical structure.

L-glutamine has a slightly different arrangement of atoms as a molecule, so differs slightly compared to glutamine, but for the purpose of our needs with gut health in relation to menopause in this article, I will use the term glutamine.
When women come onto my 12 week programmes, they have the option of listening to my new Gut Health module. Most of them do – simply because our menopause transition is a vulnerable time for changing gut health as many of you may have discovered as I did.
Oestrogen receptors (ERs) are expressed in intestinal epithelial cells, and oestradiol regulates epithelium formation and tight-junction function (Braniste, Leveque et al., 2009). It’s no surprise to me that numerous women find that they arrive in menopause and they start to experience symptoms of irritable bowel, bloating, diarrhoea, constipation, or both!
However, there’s more to the causes of inflammation in the gut apart from menopause, that we have to be mindful of as well.
Too much stress in our lives, chronic insomnia, severe shock and trauma and conditions whereby women are exercising excessively, or doing too much fasting, and those with a high-fat diet all affect the plasma concentration of Glutamine (and L-glutamine), significantly reducing levels.
Food allergies, alcohol and antibiotics all negatively affect the epithelial tight junctions too.
I wonder how many of these factors you can tick off?

The accummulation of numerous factors impact on your gut health, your sleep quality and vice versa. Over time, these impact the hardening of your arteries.
As such, the normally tight epithelial junctions become severely compromised. This causes the barrier to become impaired and inflammatory molecules, such as endotoxins, can reach the different organs via the circulation, playing a role in the pathogenesis of non-intestinal disorders, such as alcoholic and non-alcoholic liver diseases, diabetes, obesity, and chronic kidney disease.
Hence, one of the nutrients to check in your diet to help turn around your leaky gut is glutamine.
Glutamine has multiple functions in helping to preserve the (gut) health of mid-life and post-menopausal women.
Glutamine is an important amino acid (protein) and is best known for its ability to serve as a source of fuel for all sorts of cells in the body – from renal epithelial cells, to nerves and immune cells, Beta cells of the pancreas and of course, both skeletal and cardiac muscle cells – glutamine is involved in glucose metabolism and maintaining your body’s acid-alkaline balance of body fluids.
For those of you doing heavy resistance training, you may also have heard of glutamine’s role in muscle building. As a supplement for body-building, the role of glutamine has been known for years, because it serves as a necessary precursor for muscle growth.
It is also known to be in many supplements marketed to athletes, because exhaustive, heavy physical training leads to a nearly 25% depletion of plasma glutamine levels. The recovery of such a glutamine deficit requires a longer period of rest and improved nutrition, as is known in the recovery of athletes experiencing over-training syndrome.
If you are an exerciser and doing heavy physical exercise (weights and/or cardio) or you have a physically active job, then please remember that during menopause when lowering oestrogen is affecting your muscles as well, this is also a vulnerable time for your gut health to become compromised.
Depletion of tissue and blood glutamine compromises your body’s defense system too. A salient point to note if any of you are recovering from covid or any of its variants.

The epithelial tight junctions constitute the major component of gut barrier function. Hence, your gut mucosa is the major site of glutamine metabolism and absorption. It therefore has a protective influence on the gastrointestinal mucosa. This is why L-glutamine/ glutamine supplements are marketed for gut health repair.
L-glutamine in supplement form raises the level of muscosal and plasma glutamine. But so too do food sources of glutamine and there are plant sources as well as animal sources.
Animal sources of glutamine include:
- Salmon and fish
- Meat and chicken
- Eggs
- Dairy products
Plant sources of glutamine include:
- Red cabbage, brussel sprouts
- Celery
- Spinach and Kale
- Chickpeas
- Parsley
- Papaya
- Fermented foods such as Miso
- Wholegrains
Ongoing insomnia and changing gut health as women transition menopause reminds us that we need to adjust our diet and lifestyle to accommodate the changes that our body is undergoing.
That’s the purpose of the MyMT™ programmes – I want you to learn what lifestyle changes to make and why they are necessary. I also want you to feel supported, so I have a fabulous community of like-minded women!
We often turn to supplements and medications (and yes, these do have a role to play in helping to turn around symptoms), however, as I discovered myself, they don’t necessarily target all of the organs around our body.
For example, our experience of changing gut health is not only linked to menopause, but also to the enormous array of societal influences from our food production, sources of stress, exercise influences and of course, the fact that as women, there has been very little research on lifestyle that specifically addresses our needs during mid-life.
Lowering oestrogen levels in our gut epithelial lining causes the tight junctions to become more permeable to toxins in our diet and the environment. The knowledge that alcohol and the consistent consumption of low-quality, high carbohydrate processed foods low in fibre, can stress and potentially harm the gut, helps us to understand that changing our diet is important to our ongoing gut health. So, too is the adequate intake of glutamine.
Considering that the intestines depend on glutamine more than other organs, stress on the gut (from numerous factors that I mentioned earlier) will require much of the glutamine circulating in the body. Glutamine is recruited to maintain gut integrity, however once glutamine stores are depleted, the intestinal lining is left even more vulnerable to cumulative damage over time. Some of you may be feeling this already.
Zinc is another nutrient that helps to heal our gut lining too (those of you with Crohn’s Disease will already know this) and I talk about this fabulous nutrient in the MyMT™ Food Guide as part of my programmes. Many foods high in zinc are also high in glutamine – a double-winner in the fight against leaky gut syndrome and other gut disorders as we begin to consciously think about our health as we age.

If you are struggling to make the lifestyle changes that will help your symptom and weight management during your menopause transition and into your post-menopause years, then it would be my privilege to support you sometime. Details are on the My Menopause Transformation website.
References:
Braniste, V., Leveque, M., Buisson-Brenac, C., Bueno, L., Fioramonti, J., & Houdeau, E. (2009). Oestradiol decreases colonic permeability through oestrogen receptor beta-mediated up-regulation of occludin and junctional adhesion molecule-A in epithelial cells. The Journal of physiology, 587(Pt 13), 3317–3328. https://doi.org/10.1113/jphysiol.2009.169300
Buford T. W. (2017). (Dis)Trust your gut: the gut microbiome in age-related inflammation, health, and disease. Microbiome, 5(1), 80. https://doi.org/10.1186/s40168-017-0296-0
Cristina Menni, Chihung Lin, Marina Cecelja, Massimo Mangino, Maria Luisa Matey-Hernandez, Louise Keehn, Robert P Mohney, Claire J Steves, Tim D Spector, Chang-Fu Kuo, Phil Chowienczyk, Ana M Valdes, Gut microbial diversity is associated with lower arterial stiffness in women, European Heart Journal, Volume 39, Issue 25, 01 July 2018, Pages 2390–2397, https://doi.org/10.1093/eurheartj/ehy226
Deters, B. & Saleem, M. (2021). The role of glutamine in supporting gut health and neuropsychiatric factors. Food Science and Human Wellness, 10(2), 149-154 https://doi.org/10.1016/j.fshw.2021.02.003.
Lenders C., Liu S., Wilmore D., Sampson L., Dougherty L., Spiegelman D., Willett W. (2009). Evaluation of a novel food composition database that includes glutamine and other amino acids derived from gene sequencing data. Eur J Clin Nutr. 2009 Dec;63(12):1433-9. doi: 10.1038/ejcn.2009.110. Epub 2009 Sep 16. PMID: 19756030; PMCID: PMC3249386.
Grenham S., Clarke G., Cryan J., & Dinan, T. (2011). Brain–Gut–Microbe Communication in Health and Disease. Frontiers in Physiology, 2 (94), 1-15. https://www.frontiersin.org/article/10.3389/fphys.2011.00094
Skrovanek, S., DiGuilio, K., Bailey, R., Huntington, W., Urbas, R., Mayilvaganan, B., Mercogliano, G., & Mullin, J. M. (2014). Zinc and gastrointestinal disease. World journal of gastrointestinal pathophysiology, 5(4), 496–513. https://doi.org/10.4291/wjgp.v5.i4.496.