Migraine is three times more common in women than in men and is the 4th leading cause of disability in women. Onset of migraine increases at menarche, with peaks in prevalence in the late 30s, and a rapid decline after menopause. While the prevalence is highest among women of childbearing age the frequency of headache and burden of migraine frequently worsens during midlife. (Pavlovic, 2020)
If you’re one of the millions of women around the world who are entering your menopause transition and have found that you are now getting migraines, then welcome, you aren’t alone.
New research reports that during both peri-menopause (an average age of 47 yrs), and post-menopause (after 51 yrs), the frequency of headaches and incidence of migraines increases and is an ongoing burden on women in midlife. With migraines being three times more prevalent in women than men of a similar age, it’s little wonder that the severity and frequency of migraines is now understood to be linked to our changing hormones in menopause.
According to the Global Burden of Disease study, migraine is the 2nd most globally disabling condition after low back pain. If you’re troubled by migraines and headaches, especially now that you’re in mid-life, you won’t be surprised by this I’m sure. But it’s not only distressing, it’s distracting.
I’ve had numerous women on my 12 week programmes who report that they have had to take time off work and/or have lost their jobs because of their migraines impacting their ability to work. Goodness knows what the home environment is like as well.
However, thanks to the ongoing research from the Women’s Health Across the Nation (SWAN) Daily Hormone Study, we know more about migraines. And using this knowledge, I’ve been able to combine it with cardiovascular and nutrition research to bring you some tips to help ease the burden of your migraines and headaches as you transition menopause.
This includes understanding that the type of exercise you do to help relieve your migraines matters as well. And whilst I don’t get regular migraines, I’ve nursed women who do and the obvious place to hide is in bed within a darkened room.
But yoga therapies have also been clinically evidenced to reduce the episodes of headaches and migraines (Kisan,et al, 2014), so I hope you are able to add this to your ‘Menopause Symptom Toolbox’ as well.

Defining your Menopausal Migraines
There are two types of migraine that affect women primarily:
- Migraine without aura (also called classic migraine).
- Migraine with aura. Aura refers to vision changes such as flashing lights, floating spots, light sensitivity and/or tingling in your hand or face).
Migraine without aura accounts for approximately 80% of women reporting migraines in peri- or post-menopause. This is why it is associated with hormonal fluctuations. Peri-menopause headaches usually occur within the 5-day window spanning the 2 days prior to menstruation to the third day of menstruation, but in post-menopause, this is categorised in the migraine literature as non-menstrual migraine. When you see your Doctor, you will be diagnosed with migraine in accordance with the International Criteria for Migraine with or without aura.

Whilst the prevalence of migraine typically declines after menopause when you are post-menopausal, with stabilisation of oestrogen down to low levels, please be aware that migraines are now known to occur more frequently in women (even those on HRT) during their post-menopause years. Furthermore, Jelena Pavolic (2020) reports that while migraines improve in the majority of women following natural menopause, these can worsen in women (the literature reports nearly 70%), if they have had surgical menopause.
Migraines are a disorder of your Central Nervous System and High Blood Pressure can make them worse.
Although the link between falling oestrogen levels and migraines has been known for over 40 years, relatively few studies have been undertaken on patterns of migraine in peri-menopause and post-menopause women. For our generation this research is important and the work of Jelena Pavlovic (NMD, PhD) in this space is welcomed.
Knowing that migraines occur due to a disturbance of the central nervous system is important. Knowing that they also occur more frequently due to stress is equally important.
But there is something that is often missing in discussions about hormonal headaches and migraines – and that is the changing nature of our blood vessels change as we lose oestrogen. If you’ve been following my blogs for a while, you will know that I’m always talking about the role of oestrogen in our blood vessels and how, during menopause, blood vessels are losing some elasticity as a normal part of ageing.
Declining levels of oestrogen also impact our nervous system. Especially our central nervous system. As the myelin sheath which forms the outer layer of your nerves adjusts to menopause, the exchange of sodium and potassium, which helps to move the electrical current along your nerves, slows down as we move through menopause.
This knowledge helps me to help you and the thousands of women on the MyMT™ programmes who mention on their health screening forms that they experience migraines or headaches and below, I share some of these tips with you.

My 3 Tips for You to Manage your Migraines:
Help your Blood Pressure to remain Low:
Women on the MyMT™ programmes learn all about dietary nitrates. The current body of evidence for potential beneficial effects of dietary nitrates on blood pressure and improved endothelial function of our blood vessels has increased year by year, thankfully. The studies to date suggest that dietary nitrate acutely lowers blood pressure in healthy humans. There are a number of potential mechanisms that occur due to eating vegetables that are higher in dietary nitrates (including beetroot and celery) including increasing vasodilation (the diameter of our blood vessels) and inhibiting platelet aggregation (clumping) as well as reducing inflammation.

Help your Eyes:
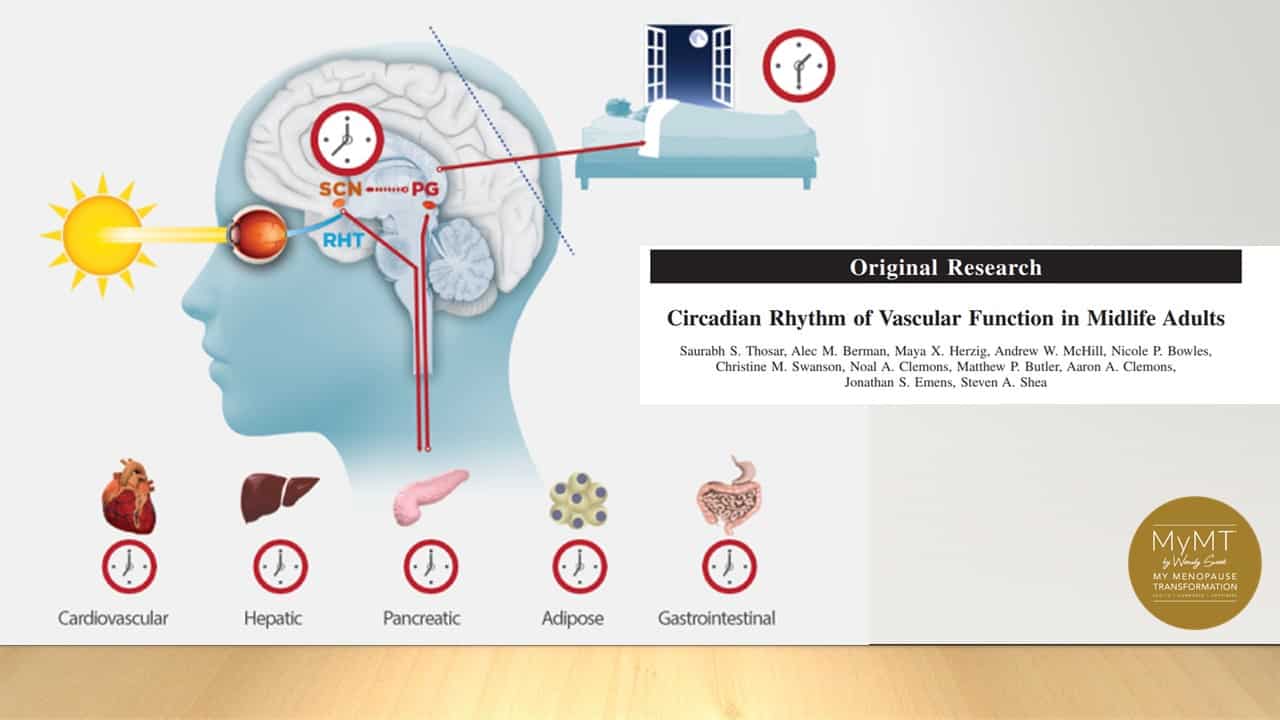
Your eyes are replete with tiny blood vessels and nerves. If you are getting migraines, then I’m sure you know about the debilitating effect that your migraine has on your eyes, but if you know that your migraines are worse in the days leading up to your period if you are peri-menopausal, then how about you work on ‘prevention’. Wear low blue light glasses if you are working on your computer and my other tip is to get natural light into your eyes during the morning. This works in better with the natural circadian rhythm of your blood vessels too.
Harness Better Breathing – this is where YOGA exercise comes into the equation.
With the knowledge that migraines are ‘more than just a headache’ and a disorder of the central nervous system (CNS), it’s important to improve your breathing. The CNS regulates heart rate, blood pressure, our response to stress and of course, temperature regulation. I’ve written numerous articles in the past about breathing better, because I want you to understand that slowing down both your heart rate and respiratory rate helps to prevent migraines.
This is why yoga therapies are also part of migraine prevention. Both aerobic exercise and yoga therapies have been found to improve endothelial function and Nitric Oxide bioavailability, which I mentioned earlier as being important for dilating your blood vessels (including your brain blood vessels) and reducing the over-activity of your sympathetic nervous system (yuor ‘fight or flight’ stress system). Research in this area of migraine management reports that because our nervous system is involved in managing the body’s response to stress, and because stress is a well-known trigger for migraines, yoga therapy decreases the stress-response.

When it comes to our symptoms in menopause we need to be proactive
Finding ways to reduce your symptoms may take more than just medications or supplements, which yes, you can also talk about with your Doctor. My focus is on helping you to action the available lifestyle science that is evidenced to help your symptoms and/or your weight. My focus in my programmes is that you understand ‘what to do’ but also, ‘why you need to do it’ – that helps you put the strategies into action (I hope!).
So, that’s what I’ve done for you – I’ve taken the best research available from a range of disciplines and put it into a step-by-step approach to turning around your symptoms over a 12 week time-frame.
All you do is to follow my plan and I have wonderful support and coaching in my private coaching community too. With two separate programs available (Transform Me or Circuit Breaker) depending on whether you desire weight loss or not, MyMT™ programs are normally available for NZ$399 each, but please do check out the MyMT website or subscribe to our newsletter to be alerted to any promotional offers.
I can’t wait to help you. My video for you to learn what the programs are about can be found below.
Dr Wendy Sweet (PhD), Member: Australasian Society of Lifestyle Medicine.
Can I help you with your symptoms?
If you are just looking for a starting point, you can purchase my online Masterclass on Menopause. This is only NZ$15 (approx. AUS$14 or UK£7.5). I hope you can join me in this powerful 2 hour webinar. The great news is that now you can watch it anytime, anywhere and even pause it whenever you like and go and make yourself a cuppa too.
References:
Hobbs D., George T., & Lovegrove J. (2013). The effects of dietary nitrate on blood pressure and endothelial function: a review of human intervention studies. Nutr Res Rev. 26(2):210-22.
Kisan, R., Sujan, M., Adoor, M., Rao, R., Nalini, A., Kutty, B. M., Chindanda Murthy, B., Raju, T., & Sathyaprabha, T. (2014). Effect of Yoga on migraine: A comprehensive study using clinical profile and cardiac autonomic functions. International journal of yoga, 7(2), 126–132. https://doi.org/10.4103/0973-6131.133891
Pavlović, J.M. (2020). The impact of midlife on migraine in women: summary of current views. Women’s Midlife Health 6, 11, 1-7.
Pavlović J.M. (2018). Evaluation and management of migraine in midlife women. Menopause. 25(8), 927-929.
Sengupta P. Health Impacts of Yoga and Pranayama: A State-of-the-Art Review. Int J Prev Med. 2012 Jul;3(7):444-58.
Tanaka, H., Dinenno, F., Monahan, F. et al (2000). Aging, Habitual Exercise, and Dynamic Arterial Compliance. Circulation, 102 (11), 1270–1275
Related Tag: Sign of Menopause


