Over 60 million women (44%) in the United States are living with some form of heart disease. This is the leading cause of death for women in the United States and can affect women at any age.
In 2021, heart disease was responsible for the deaths of 310,661 women— or about 1 in every 5 female deaths. [CDC, 2023]. In the United Kingdom, heart and circulatory diseases cause a quarter of all deaths and to date, around 3.6 million females in the UK are living with cardiovascular disease. [British Heart Foundation, 2023]
Women’s health and ageing research is replete with cardiovascular disease studies. The declining health of our mother’s generation have paved the way for this type of research in older women. For many women, menopause is the start of their changing heart health … but here’s the thing that our mother’s generation didn’t know – it doesn’t have to be this way.
Menopause is the time when wmany women are most at risk of high blood pressure and changing heart health and researchers now understand that the mid-life years are the time to change how we look after ourselves. Otherwise, hot flushes, poor sleep, hypertension and aching joints may continue into the post-menopause years, contributing to worsening cardio-metabolic health.
With women’s death rate from heart disease in America nearly eight times higher than death rates from cancer, and New Zealand, Australia and the UK leading the world in heart disease incidence, increasing evidence indicates that hormonal changes in menopause may also be involved (Maas, 2020).
How women choose to manage their menopause symptoms with medications is entirely up to them.
But my own experience, is that many women don’t realise that drug treatments alone may not keep them healthy – especially when it comes to understanding the powerful connection between the menopause transition and age-related changes to the endothelial lining of their blood vessels.
Over 30 years ago in the early 1990’s, when I was a former ICU nurse, every now and again, there would be a call to go and help-out the busy nurses in the Coronary Care Unit.
At the time, I didn’t give a thought to how many of the patients lying in beds hooked up to cardiac monitors were women who had just arrived in menopause or post-menopause.
But they were – and now that I’m in post-menopause myself and with my women’s healthy ageing studies leading me down the rabbit-hole about the effect of declining oestrogen on other organs around the body, including cardiac muscle and blood vessels, these memories make sense.
Women in their menopause transition and those already in post-menopause are at increased risk for changing heart health as they age.
Whilst both weight gain and poor sleep patterns affect post-menopause heart health, research also suggests that Vitamin D exerts a powerful influence on cardiovascular health in menopause, including in the mechanisms leading to arterial stiffness. (Al Mheid et al., 2011; Thompson et al, 2023)
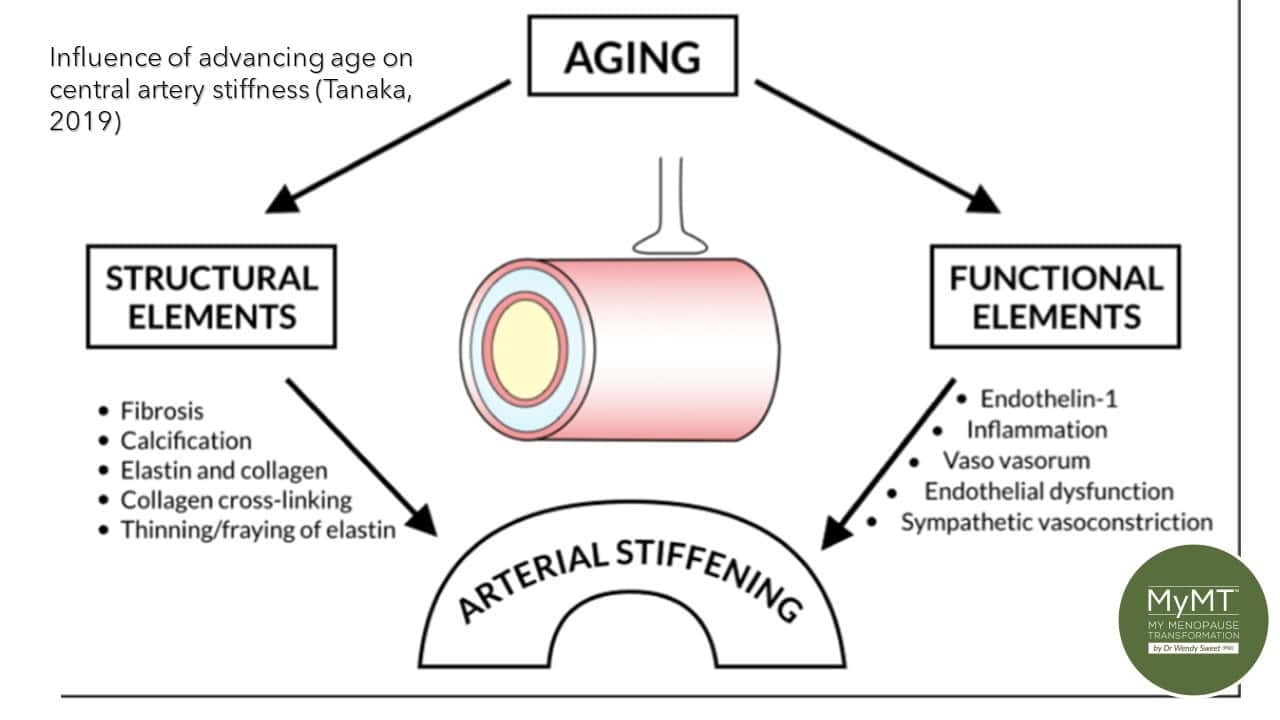
What is Arterial Stiffness?
You’ve probably already heard of the concept of ‘hardening of the arteries’ and the link to changes in the walls of blood vessels due to inflammation and obstructive lesions. However, as more and more research has been conducted, the term ‘arterial stiffening’ has emerged, especially as this relates to women’s cardiovascular status as they age.
Arterial stiffness relates to alterations of the internal wall of the blood vessel, which can cause reduced distensibility of the arterial wall. Essentially the walls become less elastic, which decreases the ability of the arteries to buffer against changing blood pressure.
This stiffening of the large arteries is the central paradigm of vascular ageing in both men and women, (Shirwany & Zou, 2010). While a number of mechanisms are known to contribute to vascular stiffness in women, especially the decline in oestrogen during, menopause, it is also known that Vitamin D status is associated with vascular or arterial stiffness too (Al Mheid et al, 2011).
What is the effect of Vitamin D on the arterial walls?
Although the link between the risk of deteriorating bone health and Vitamin D status is well known in women, low Vitamin D also confers vascular risk too.
According to recent studies, Vitamin D helps to modulate the endothelial lining of the blood vessels, providing protection against inflammation due to ageing. As such, the study by Al Mheid et al (2011) suggests:
“Our findings of increased arterial stiffness and endothelial dysfunction in indivduals with low 25-OH D, … might predispose individuals to a higher risk for the development of hypertension, cardiovascular disease and adverse events.” (p. 6).
Shift Workers and Vitamin D Levels:
In many diseases of older age for both men and women, there is often low Vitamin D status which commences in mid-life. For women, the change in Vitamin D status generally begins during menopause as the skin is replete with oestrogen receptors which are losing the role of oestrogen.
Furthermore, if you have clients who are night shift-workers, such as many nurses, low Vitamin D levels are often the start of a slippery slope towards more immune health changes and increased inflammation building up in the body, including depression.
Part of the reason for lower Vitamin D levels hitting women during menopause, is our changing oestrogen levels.
Oestrogen receptors can be found all over our body, including in our epithelial tissue (skin), so during our menopause transition, when we begin to lose oestrogen receptor cells, it’s not just the ovaries that are affected.
Other oestrogen-attracting cells are too. What this means is that women (both fair-skinned and dark-skinned women) don’t synthesise (produce) Vitamin D very well in menopause. It also means that night shift-workers get a double-whammy of losing oestrogen and losing exposure to Vitamin D because they have less available sunlight hours if they sleep all day.

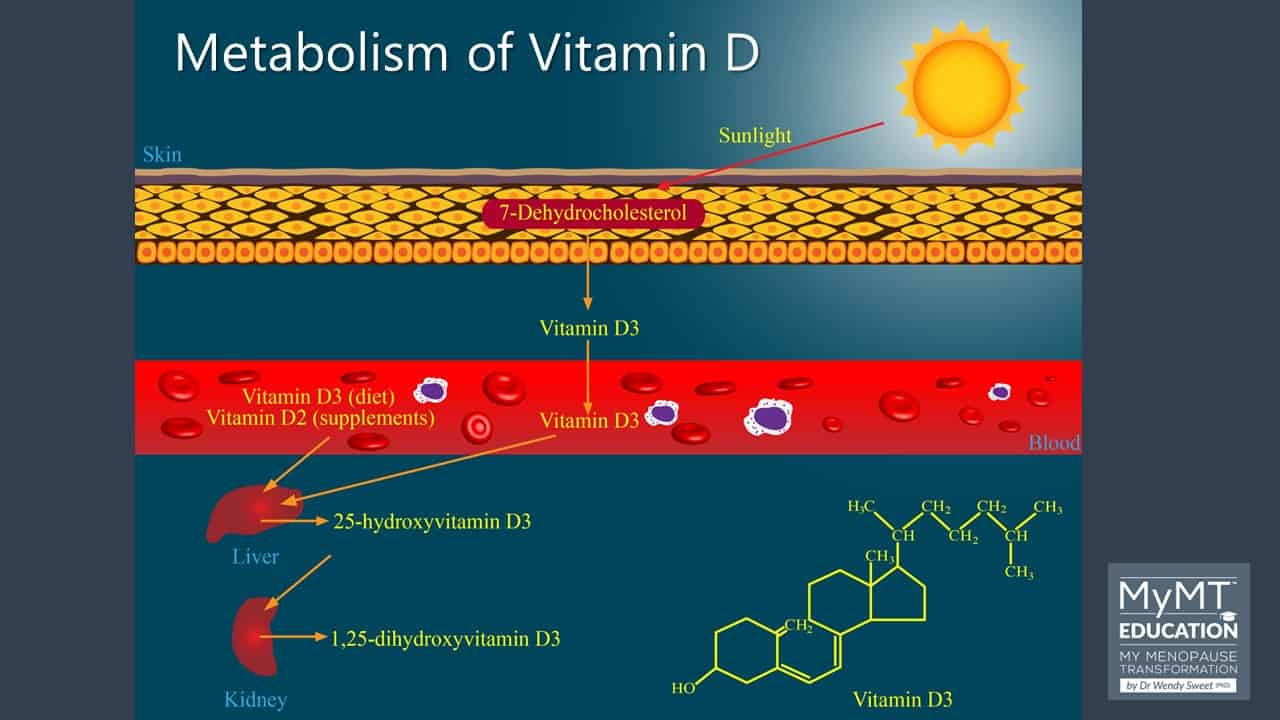
Unlike other essential vitamins that must be obtained from food (these ‘essential vitamins’ aren’t made in the body, so we need to source them from food), Vitamin D can be synthesised in the skin through a photosynthetic reaction triggered by sunlight.
The efficiency of this production is reliant on exposure to sunlight directly on our skin and we produce Vitamin D3 which then undergoes additional transformation (in the presence of oestrogen) to 25-hydroxyvitamin D, which is the major form of Vitamin D that circulates in our bloodstream.
Between the skin cells and the liver, our body carries out this transformation, but another transformation occurs in the kidneys forming 1, 25 (OH)D.
By now, Vitamin D has become a hormone and it goes on to accumulate in the intestine, where it enhances calcium and phosphorous absorption – controlling the flow of calcium into and out of bones to regulate calcium-bone metabolism.
Over 1000 different genes governing virtually every tissue in the body are now thought to be regulated by Vitamin D3.

One of the most important strategies for the women I coach on both of the MyMT programmes is for them to get their Vitamin D levels tested if possible.
If these are low, then this is one of the only supplements that I encourage them to take – especially for women doing night-shifts and those who are in their winter months.
It’s far more important for women to get this Vitamin from good food sources as well – in fact I think it is even more important than any menopause supplement that is on the market (which often don’t have good scientific research to qualify the effectiveness of the supplements).
I hope that you can also encourage your menopausal and post-menopausal ladies to get their Vitamin D levels checked with their Doctor. To me, it’s one of the most important lifestyle strategies that we can encourage!
Don’t forget that I have more information for you on Vitamin D in the MyMT™ Practitioner Course – Georgia has opened up the pre-registration for the January intake, so don’t forget to register your interest HERE.

References:
Al Mheid I, Patel R, Murrow J, …, Brigham K, Quyyumi A. Vitamin D status is associated with arterial stiffness and vascular dysfunction in healthy humans. J Am Coll Cardiol. 2011 Jul 5;58(2):186-92.
Avolio A. Arterial Stiffness. Pulse (Basel). 2013 Apr;1(1):14-28. doi: 10.1159/000348620.
Benefits of sunlight: A bright spot for human health. Environmental Health Perspectives, (2008). 116(4), 161-167.
Lehnert M. et al. (2018). Vitamin D supply in shift working nurses. Chrono-biology International.
Shirwany NA, Zou MH. Arterial stiffness: a brief review. Acta Pharmacol Sin. 2010 Oct;31(10):1267-76.
Thompson B, Waterhouse M, English DR, McLeod DS, Armstrong BK, Baxter C, Duarte Romero B, Ebeling PR, Hartel G, Kimlin MG, Rahman ST, van der Pols JC, Venn AJ, Webb PM, Whiteman DC, Neale RE. Vitamin D supplementation and major cardiovascular events: D-Health randomised controlled trial. BMJ. 2023 Jun 28;381:e075230. doi: 10.1136/bmj-2023-075230.