If you added up all the nights in the week that you lie awake between 2-4am, how many would that be? Is it 5 or more? I’m asking you this, because when I’ve presented my Masterclass on Menopause seminars over the years, this is the question that women groan at the most. And asking that question always gets a show of hands. Hundreds of women are losing precious immune-boosting sleep as they go through menopause and for those who are avid exercisers, they don’t seem to understand that not sleeping means that they aren’t recovering from all of the exercise they are doing too – many of these women find that their hot flushes have become worse, their weight is going up and they are confused as to why. Yes, I was that woman too.
I remember only too well what it feels like not to sleep night after night. I know myself that the minute you’re awake, your brain starts going into ‘busy-mode’. If your phone is beside your bed, you look at it or you get up and do some work or you just lie there tired trying to will yourself to go back to sleep. The clock spins around another hour. When you do finally get back to sleep it seems like it’s only minutes before the alarm goes off and another exhausting day begins. What we fail to fully realise, is that when we aren’t sleeping, the belly fat starts to creep on as well. Some of you may gain up to 2 kg a week.

Modern science confirms that when we don’t sleep all night, especially between the crucial fat-burning hours of 2-4am, then we don’t lose weight. However, the double-whammy for women in their menopause transition, is that this interrupted sleep also causes more hot flushes throughout the day and leaves many women sweating throughout the night. It’s tough.
When you aren’t SLEEPING all night, you aren’t getting enough secretion of two other important hormones necessary for repairing and healing your body. Growth Hormone and Testosterone.
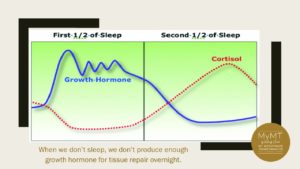
These two hormones are crucial for repairing muscle and restoring your immune system. This is why interrupted sleep in menopause throws our muscle-healing and fat-burning capability out the door. It’s also why many of you who undertake lots of exercise but you aren’t sleeping, may develop restless legs, aching joints and fatigued muscles, or you experience recurring injuries which fail to heal.

When we aren’t sleeping properly, and we aren’t recovering, then this impacts one of our stress hormones called cortisol. When cortisol levels stay high, this prevents overnight fat-burning and muscle repair. This is why the most powerful thing I do for you when you come on board into the MyMT™ programmes, is to get you sleeping all night. If you aren’t sleeping well, then this is the first breakthrough you need to focus on for halting any further fat-gain as well as for helping you hold onto your precious muscle as you move through menopause. We need our muscle to help us to boost our metabolism and burn fat. This occurs in small mitochondrial cells which store oxygen. Loss of muscle from not sleeping also means loss of mitochondria and a change in our metabolism to fat-gain, not fat-loss.

Un-raveling the science of not sleeping as we transition into our new hormonal environment in menopause took me hundreds of hours of study. But I was so determined to understand why I wasn’t sleeping, because I knew from the emerging weight loss science, that sleep and fat loss go hand in hand. Even more than exercise and different dieting regimes. Add to this, our changing hormonal environment in menopause and the subsequent loss of muscle as we age (called sarcopenia) and it becomes a ticking time-bomb for un-necessary cardiac and metabolic health changes that our mother’s generation have already discovered.
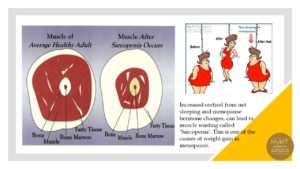
Although we kind of get by on a day-to-day basis without sleep, the issue for me and millions of women, is more about the accumulation of loss of sleep and the effect this has on our weight and our health. Not sleeping leads to ongoing inflammation in our muscles, joints, liver, gut and heart. What’s more, the increasing inflammation can send us into the cascade of chronic health changes that hit us in our post-menopause years, including auto-immune health problems.
I still remember when I couldn’t sleep night after night. I was up and down like a yo-yo and it didn’t help that hubbie was lying there snoring blissfully unaware of my despair. The supplements didn’t help nor did the HRT. Although I knew that not sleeping is the slippery slope to fibromyalgia and other auto-immune diseases, the one I was most concerned about, was the weight gain. This is because when we don’t get our deep, healing sleep, our hormones that help us to burn fat overnight become disrupted too.
Scientists divide sleep into two major types: REM (rapid eye movement) sleep or dreaming sleep, and non-REM or quiet, healing sleep. Sleep specialists have called non-REM sleep “an idling brain in a movable body.” During this phase, thinking and most bodily functions slow down, but movement can still occur, and a person often shifts position while sinking into deeper stages of sleep. When we go to bed and start to fall asleep, both phases last around 4 hours or more.
After your REM sleep, comes your deeper sleep, or your non-REM sleep. This is characterised by slow brain waves called delta waves. When your brain slows down, you allow your body to enter deep sleep. Breathing becomes more regular. Blood pressure falls, and the pulse slows to about 20% to 30% below the waking rate. The brain is less responsive to external stimuli, making it difficult to wake up. This deep sleep is really important for us to have, especially during menopause, because this is the time that your body heals, renews and repairs cells and tissues. It’s also the time that your body fat-burns and regulates metabolism.

According to the Harvard Sleep Report (2017), researchers have also detected increased blood levels of substances that activate your immune system, raising the possibility that deep sleep helps the body defend itself against infection. Just as deep sleep restores your body, scientists believe that REM or dreaming sleep restores your mind, perhaps in part by helping clear out irrelevant information. Blood flow is directed less toward your brain, which cools measurably. At the beginning of this stage, the pituitary gland releases a pulse of growth hormone that stimulates tissue growth, muscle repair and overnight fat-burning.
So, herein lies the problem. If we are lying awake between 2 and 4am, then this release of growth hormone does not reach the threshold it needs to for healing, repairing, restoring and fat-burning.
When growth hormone is low, our blood sugar hormone called insulin remains high. So too, does another stress hormone called cortisol. The combination of high insulin and high cortisol competes with your sleep hormone, called melatonin which is low as well. The lower that melatonin is overnight, the more awake you feel. The more awake you feel, the busier your brain …. night after night, it happens … and over time, your brain and your hormones have reached their ‘new normal’. It becomes routine for you to be awake at night. The weight creeps on despite all that exercise and dieting.
The result? Yes, you already know it – foggy brain, fatigue, loss of motivation, irritability and of course, weight gain. As our fat cells go into survival mode, they begin to store excess oestrogen, leading to a condition called ‘oestrogen dominance’.

If you are putting on weight or you are feeling constantly cranky, irritable and exhausted, then please let me help you turn this around. Women on my 12 week programmes (there are two different ones depending if women are overweight or not), love their learning in the first online module they receive, which is simply called ‘SLEEP ALL NIGHT’. For those with poor gut health, they also love discovering that our gut is also on a 24 hour night/day rhythm, so as they learn to sleep all night, their gut health starts to improve too.

What women on the MyMT programmes discover, [as I did myself], is how to turn around their Circadian Rhythms to match their changing hormonal levels during menopause. The term ‘Circadian’ means “about a day.” This internal clock, which gradually becomes established during the first months of life, controls the daily ups and downs of biological patterns, including body temperature, blood pressure, and the release of hormones. Circadian rhythms make people’s desire for sleep strongest between midnight and dawn, and to a lesser extent in mid-afternoon. Our changing menopause hormones cause disruption to our normal circadian rhythms, so as we transition into or through menopause, then it’s really important to restore this biological rhythm and make adjustments to get us back sleeping all night. Whilst a lot of information about sleep has emerged recently, much of this is not focused on mid-life women specifically nor on the specific gut hormones that also become affected in menopause.

If we don’t turn around our sleep in mid-life, then I’m always telling women, that this will then become their ‘new normal’, because over time, our brain and body start to read this 3am ‘awake’ period as routine. When this happens, your other hormones start to adjust and you accumulate more fatigue, muscle soreness, headaches, weight gain and more. Your immune health suffers and you keep stacking on the belly-fat – despite all the exercise you are doing or any new diet that you are on. That’s because your Circadian Rhythm affects nearly every organ in your body.
Whilst 2020 has certainly emerged as a year of challenges for all of us with the pandemic and I know that many of you are experiencing extraordinary changes in your life, I hope that you might be able to join me. Whilst the Covid-19 special pricing of NZ$199 has ended now, I still want to support you, so there is still a NZ$50 SAVING on the programme pricing. This makes is NZ$349 [AUS $235 and UK£130]. Please use the promo code MyMT2020 when you select the programme that best suits you.
 Dr Wendy Sweet, [PhD] Women’s Healthy Ageing Researcher & MyMT Founder & Coach. Member: Australasian Society of Lifestyle Medicine.
Dr Wendy Sweet, [PhD] Women’s Healthy Ageing Researcher & MyMT Founder & Coach. Member: Australasian Society of Lifestyle Medicine.

References:
Carr, M. (2003). The Emergence of the Metabolic Syndrome with Menopause. The Journal of Clinical Endocrinology & Metabolism 88(6):2404–2411
Davis, S., Castelo-Branco, C. et.al. (2012). Understanding weight gain at menopause. Climacteric, 15: 419–429.
Harvard Health Report (2017). Improving Sleep. Harvard Health Publication
Geddes, L. (2019). Chasing the Sun: The new science of sunlight and how it shapes our bodies and minds. London: Profile Books.
Nyberg, S., Singh-Manoux, A., Pentii, J. et al. (2020). Association of healthy lifestyle with years lived without major chronic diseases. JAMA Inernal Medicine Online.
Reinke H. & Asher G. (2017). Circadian clock control of liver metabolic functions. Gastroenterology, 150: 574–580.
Rizzi, M. et al. (2016). Sleep Disorders in Fibromyalgia Syndrome. Journal of Pain Relief, 5:2, 1-5
Sharma, S. & Kavuru, M. (2010). Sleep and Metabolism: An Overview. Int. Journal of Endocrinology, Article ID 270832, 1-12.
Woods, N. et al. (2009). Cortisol Levels during the Menopausal Transition and Early Postmenopause: Observations from the Seattle Midlife Women’s Health Study. Menopause, 16(4): 708–718.


