I said that statement above to my husband this morning – “You know all I wished for in my early 50’s was to sleep all night and lose the weight that exercise and dieting wasn’t shifting.” We were out walking to the local produce shop during Week 6 of lock-down here in New Zealand and met a lady whom we used to see at our local coffee shop. She was on her way there with her teen-age daughter. A brief conversation ensued at the obligatory 2 metre distance. We chatted away and talked about how she was getting on. “If I could sleep and lose my weight I’d be happier” she laughed. 5kgs had gone on during April’s lockdown she shared. This morning she was trying to walk it off.
I didn’t have the heart to tell her that in order to lose her menopause weight, what she needed to do was to sleep all night.
My increasing weight gain in my late 40’s and early 50’s frustrated me. The exercise wasn’t working and nor were the ‘diets of the day’. From my doctoral studies and years of lecturing, I also knew that night after night of not sleeping was the slippery slope towards worsening cardiac and metabolic health as women get older. Not getting enough sleep makes you more likely to gain weight, according to a review article in the journal Obesity that analyzed findings from 36 studies. The link appears to be especially strong among women during menopause. Lack of sufficient sleep tends to disrupt hormones that control hunger and appetite, and the resulting daytime fatigue often discourages you from exercising or eating healthily. How I remember those days so well!

For women aged 52-65 years, weight gain is one of their major health concerns reports the Women’s Health Program at Monash University in Melbourne, Australia (2012). I’m not surprised. Since we entered our 20’s in the 1980’s, the prvelance of obesity has more than doubled and of these, over 300 million women were obese (i.e. have a body mass index [BMI] of over 30 kg/m2). Our western lifestyle is part of this, as is decreased physical activity, but for those going into their next stage of life, the hormonal millieu of menopause, impacts on this weight gain too. That includes the chaos that ensues with our sleep.
That’s why, if you are on popular diets or exhausting exercise to try to lose your menopause weight, but you aren’t sleeping, then sorry, but you aren’t fat-burning. It’s why you end up with your weight yo-yo-ing all over the place. Just as mine did too.
 There is a biological reason why you’re not sleeping well – wakefulness, light sleeping and insomnia (not being able to get back to sleep) is linked to your changing reproductive hormones during menopause. But here’s the thing – lack of sleep really is a big deal for your health as you age.
There is a biological reason why you’re not sleeping well – wakefulness, light sleeping and insomnia (not being able to get back to sleep) is linked to your changing reproductive hormones during menopause. But here’s the thing – lack of sleep really is a big deal for your health as you age.
Not sleeping night after night,
- increases your hot flushes,
- disrupts your blood sugar hormone called insulin
- worsens forgetfulness
- reduces muscle recovery from exercise
- keeps your body in ‘stress’ mode which increases storage of fat in the abdominal area
- changes your heart health and blood pressure.
Not sleeping is a big deal for your health as you move through menopause – especially if you are putting on weight.
We all know how night after night of insufficient sleep makes you feel. You become so distracted with your fatigue that you give up exercise, you can’t get your work done and eventually, during menopause, you might notice that your hot flushes and sore joints get worse as well. These symptoms are also linked to your menopause insomnia because not sleeping leads to increased inflammation building up in your cells and tissues too. (Harvard Health Sleep Report, 2017). It’s this inflammation that sends us into the cascade of adrenal, thryoid and blood glucose changes that hit us in our post-menopause years and mess up our metabolism as we age.

How your lack of sleep leads to menopause weight gain:
I still remember when I couldn’t sleep night after night. I was up and down to the loo, making cups of tea, reading and even doing some work. I tried every strategy that I had been told about. The supplements didn’t help, nor over time, did the HRT.
Although I knew that not sleeping is the slippery slope to fibromyalgia and other auto-immune diseases, the one I was most concerned about was the weight gain.
This is because when we don’t get our deep sleep, which is our healing sleep, our hormones that help us to burn fat overnight (insulin and cortisol) become disrupted too. Being awake keeps these two hormones higher than they should be. When these hormones remain high, our body goes goes into ‘distress’ and we store more fat in our fat cells which are either, more highly distributed around our mid-section or around our thighs mentions researcher, Molly Carr, [2003].
“Two patterns of body fat distribution have been observed. The accumulation of fat centrally, as intraabdominal fat (android or apple shape) and the accumulation of fat in the gluteo-femoral region (gynoid or pear shape).” Both have their health risks during and after menopause.
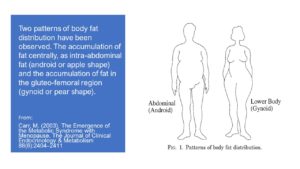
But there are other conditions that cause weight gain in menopause and none more so, than if you’ve had a hysterectomy or just had your ovaries removed (oophrectomy). If this is you, then please take note that studies on oophrectomised mice show that fat tissue (adipose tissue) becomes more inflamed and fatty liver can result as well. I guess some of you who have had a hysterectomy, might already understand this with your weight going up, not down. When I met Elaine in Sheffield during my UK lecture tour earlier this year before the world headed into Covid-chaos, she mentioned that she had no idea how much her weight would balloon after her hysterectomy, but now she realises that not sleeping during peri-menopause was contributing to this weight gain too.

As I tell women on my 12 week programmes, “getting your sleep sorted is the foundation to improved weight management and cardiac health as we age.” When I was so confused about my own weight gain, I had no idea about this either, until I looked into it as part of my women’s healthy ageing studies.

Why aren’t we sleeping?
Unraveling the science of not sleeping as we transition into our new hormonal environment in menopause took me hundreds of hours of study, but I was so determined to understand why I wasn’t sleeping.
Nobody told me it was all to do with the clash between my changing hormones in menopause as part of natural ageing and my diet and exercise, which was more suited to my ‘younger-self’ and not someone going through menopause.

Just as deep sleep restores your body, scientists also know that REM or dreaming sleep restores your mind, perhaps in part by helping clear out irrelevant information. A very important task for a generation of women with a lot going on in their lives still! When we get this deep, restorative sleep (between 2 and 4am), blood flow is directed less toward your brain, which cools measurably. At the beginning of this stage, your pituitary gland releases a pulse of growth hormone to stimulate tissue growth and muscle repair.
If we are lying awake between 2 and 4am, then this release of growth hormone does not reach the threshold it needs to for healing and repairing our body. This is why I hear from so many women who are avid exercisers; they don’t understand that their sore muscles and joints are due to not just low oestrogen, but also not sleeping!
We need to sleep all night again in order to reduce our joint pain as well as allow our body to recover from bouts of exercise.
Sleep is vital for activating our immune system:
Deep sleep activates our immune system. So, for those of you doing more vigorous exercise, then not sleeping may be causing your performance to drop and your muscles and joints to remain sore for longer after training. It’s the same for over-trained athletes who don’t sleep well. Their performance gradually drops off followed my their motivation too. What happens next is a series of changes in the levels of stress hormones that cause our sleep hormone, melatonin to decline further than it has already.

For ex-Les Mills Group Fitness Instructor, Tineke, understanding this was crucial to her weight loss success.

Sleep is vital for regulating insulin, cortisol and melatonin levels:
The other concern is that when we aren’t sleeping well, our blood sugar hormone called insulin, remains high. So too, does our chronic stress hormone called cortisol. A high sugar diet and increased stress also messes up the production of melatonin, our precious go-to-sleep hormone.
This powerful combination of high insulin and high cortisol not only prevents your overnight fat-burning, but the presence of these hormones at higher levels before you go to bed competes with your sleep hormone called melatonin. If you are in menopause, then watch how much alcohol or sweet treats you have in the evening too. So many women don’t understand that alcohol converts to oestrogen and is stored in our fat cells too.
Our melatonin hormone levels are important. The lower that melatonin is before you go to bed and the lower it stays overnight, the more awake and restless you are during the night. The more awake you feel, the busier your brain and the more hot flushes you have … night after night it happens and over time your brain and your hormones are now reading this as your ‘new normal’. Every day then becomes a marathon to get through.

As many of you already know – the result is daily fatigue, exhaustion, irritability, depression, sore joints and with your insulin levels all mixed up overnight, the weight starts to increase around your belly or around your thighs too.
That’s why in the MyMT™ ‘Transform Me’ weight loss programme the first module you listen to is simply called ‘Sleep All Night’. Without this precious sleep, your body doesn’t burn fat.

Not sleeping has such a negative effect on our health as we age including on our liver and gut health.
If you are putting on weight or you are feeling constantly cranky, irritable and exhausted, then please let me help you turn this around. Women on my online 12 week programmes love their learning in the first online module they receive, which is simply called ‘SLEEP ALL NIGHT‘. For those with poor gut health, they also love discovering that our gut is also on a 24 hour night/day rhythm, so as they learn to sleep all night, their gut health starts to improve too.
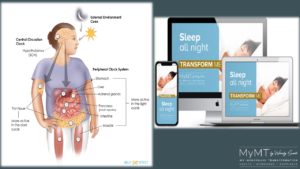
One of the powerful strategies that women on my programmes discover is the importance of our Circadian Rhythms and how to adjust these to specifically match their changing hormonal levels during menopause. The term ‘Circadian’ means “about a day” so our circadian rhythms are daily fluctuations in our biology that can become messed up as we transition through menopause.
This internal clock, which gradually becomes established during the first months of life, controls the daily ups and downs of biological patterns, including body temperature, blood pressure, and the release of hormones which control all of our body’s workings – this includes our weight management.

Circadian rhythms make people’s desire for sleep strongest between midnight and dawn, and to a lesser extent in mid-afternoon. However, our changing menopause hormones cause disruption to our normal circadian rhythms, so as we transition into or through menopause, then it’s really important to restore this biological rhythm and make adjustments to get us back sleeping all night. If we don’t, then over time our brain and body start to read this 2-3am ‘awake’ period as ‘normal’. This is why food-timing is important as well and I get all the women who join me to focus on changing the time of their evening meal to better suit their circadian rhythm which controls digestion overnight.

Certain brain structures and chemicals produce the states of sleeping and waking. Levels of melatonin begin climbing after dark and ebb after dawn. This powerful hormone induces drowsiness, and scientists believe its daily light-sensitive cycles help keep the sleep/wake cycle on track.
As we enter our mid-life years, these levels of melatonin decline as oestrogen starts to decline. This means that our deep sleep continues to diminish. Night-time awakenings become more frequent and last longer. Waking after about three hours of sleep is particularly common and many women experience hot flushes, night sweats or want to get up and have a pee (yes, we have oestrogen receptors in our bladder as well). But the other main issue is weight gain.
Is it time to get control over your weight and your sleep?
When I began to look into our menopause symptoms as part of my women’s healthy ageing studies, I began to understand that our menopause transition is a natural transition that all women go through. Menopause is therefore, not the problem. We all go through it. The problem is that for millions of women, is that we are continuing to go about our daily life as if we aren’t in menopause. But we are! And when we make some simple lifestyle changes we can turn around the chaos naturally. With my 12 week programme, this all starts with turning around your sleep.
During the pandemic, I have had the MyMT™ Transform Me 12 week programme on sale with NZ$100 off. This makes it NZ$349 which is the lowest price it has ever been, but it is my way of supporting you all during this time. There are also part-payments you can choose from and the promo code to use on any BUY NOW button is JOIN MYMT. In Australia and New Zealand as we move back to a more ‘normal’ way of life, the price will revert at the end of May. For those of you in the UK, I will watch how you are getting on and may leave this pricing for a little bit longer if your lock-down continues. Over 12 weeks you discover my plans and strategies how to turn around your sleep, liver health, hot flushes, nutrition and improve your energy again. All of this is accessed in your exclusive member area on the website.
If you aren’t sleeping and/or putting on weight during or after your menopause transition, then I hope you can join me. Women around the world call it ‘life-changing’. I tell you all about it in the short 6 minute video below.

BOTH programmes come with my BONUS MyMT™ FOOD GUIDE – packed full of the most relevant food information and recipes that I have specifically evidenced against women’s healthy ageing nutritional studies. I became so confused about nutrition, despite lecturing on nutrition at university, but then I began to understand that the information that was available at the time, was not suited to our age and stage in menopause – and no, the popular Keto or Paleo diets are not what I teach either. I teach you how to reduce inflammation in your joints, gut and muscles by using nutrition evidenced from women’s healthy ageing studies and this includes the Mediterranean Diet, Heart Health and Longevity science as well. As soon as you join me, this fabulous Food Guide is loaded up into your exclusive member area for you.

Dr Wendy Sweet, PhD/ MyMT™ Founder/ Member: Australasian Society of Lifestyle Medicine.
“Putting menopause into wellness, not sickness for over 2000 women around the world. Join me when you can.”
References:
Carr, M. (2003). The Emergence of the Metabolic Syndrome with Menopause. The Journal of Clinical Endocrinology & Metabolism 88(6):2404–2411
Davis, S., Castelo-Branco, C. et.al. (2012). Understanding weight gain at menopause. Climacteric, 15: 419–429.
Harvard Health Report (2017). Improving Sleep. Harvard Health Publication
Geddes, L. (2019). Chasing the Sun: The new science of sunlight and how it shapes our bodies and minds. London: Profile Books.
Nyberg, S., Singh-Manoux, A., Pentii, J. et al. (2020). Association of healthy lifestyle with years lived without major chronic diseases. JAMA Inernal Medicine Online.
Reinke H. & Asher G. (2017). Circadian clock control of liver metabolic functions. Gastroenterology, 150: 574–580.
Rizzi, M. et al. (2016). Sleep Disorders in Fibromyalgia Syndrome. Journal of Pain Relief, 5:2, 1-5
Sharma, S. & Kavuru, M. (2010). Sleep and Metabolism: An Overview. Int. Journal of Endocrinology, Article ID 270832, 1-12.
Woods, N. et al. (2009). Cortisol Levels during the Menopausal Transition and Early Postmenopause: Observations from the Seattle Midlife Women’s Health Study. Menopause, 16(4): 708–718.



